By Marcello Cherchi, MD PhD
For patients
In simple terms, the word “ototoxicity” broadly refers to the damaging (toxic) effects that various chemical agents (such as therapeutic drugs or industrial compounds) can have on hearing and balance.
While there is substantial literature on this topic, there is also substantial controversy. Some drugs are better documented to have toxic effects on balance and/or hearing. For other drugs the connection is less clear.
The most important first step is to identify whether there are measurable deficits in balance and/or hearing. Your doctor may try to figure this out from a variety of auditory tests and vestibular tests.
The vast majority of cases of ototoxicity are irreversible. Nevertheless, if objective evidence of auditory and/or vestibular deficits are found in a patient in whom there is reasonable suspicion that potentially ototoxic agents may be contributory, then if medically feasible it is reasonable to stop the offending medication, and avoid its use in the future.
In some life-threatening diseases, current treatments have known ototoxicity, but withholding the treatment may not be a realistic option, so patients and their practitioners treat in full awareness of this risk. The diseases in question are usually certain kinds of infections (that require treatment with aminoglycoside antibiotics) and certain forms of cancer (that require treatment with platinum-based chemotherapeutic agents).
For clinicians
Overview
Ototoxicity refers to damage of otologically-mediated auditory and/or vestibular function by a chemical compound. Drug-related ototoxicity is nearly always undesirable (with the main exception being purposeful ablation of labyrinthine function by transtympanic gentamicin injection). An extraordinarily broad range of chemical compounds have been documented to have potential ototoxicity, including various anti-microbial agents, anti-arrhythmic agents, immunosuppressants, anti-neoplastic agents, diuretics and others. Various attempts at monitoring cochlear and vestibular ototoxicity, protecting against ototoxicity, and treating ototoxicity have been attempted, without clear success.
Definition
For purposes of this discussion we define ototoxicity as damage of otologically-mediated auditory and/or vestibular function by a chemical compound.
We use the phrase “otologically-mediated” to delimit the topic to damage of the labyrinth and/or vestibulocochlear nerve. We specifically exclude damage of other anatomical structures. Thus, for example, chronic alcoholism can damage the cerebellum; one may say that a chemical (ethanol) has led to imbalance, the main structure affected by the chemical is the cerebellum, not the labyrinth or vestibular nerve.
We use the phrase “chemical compound” to include prescribed medications (drugs), as well as illegal substances (e.g., marijuana (Qian & Alyono, 2020)) or misused chemicals (e.g., inhaled toluene). We also use this phrase to excluded non-chemical otologic damage, such as radiation toxicity.
Is ototoxicity always bad?
In short, ototoxicity is nearly always a bad thing, with very few exceptions. The main exception in otoneurology is when gentamicin is intentionally administered transtympanically for chemical ablation of the labyrinth as treatment for Ménière’s disease.
Agents implicated
Hundreds of drugs and other chemicals have been implicated as ototoxic. It is impractical to review these all, but a sense of the breadth can be conveyed by the following diagram (Watts, 2019).
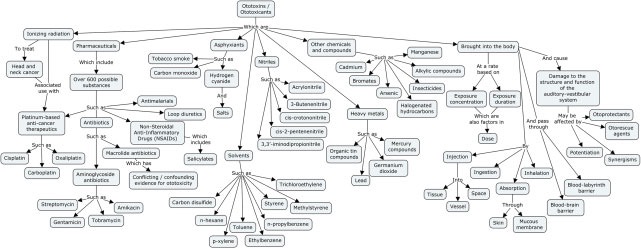
The main regulated ototoxic medications encountered in clinical practice include aminoglycoside antibiotics (usually gentamicin) and platinum-based chemotherapeutic agents (usually cisplatin), but there are many other agents for which ototoxicity has been implicated though less well substantiated. PubMed search with the term “ototoxicity” returns >6000 hits.
Anti-microbial agents: Aminoglycoside antibiotics
Aminoglycoside antibiotics are well-documented to be ototoxic (Henley & Schacht, 1988; Huth, Ricci, & Cheng, 2011; Rizzi & Hirose, 2007; Ruhl et al., 2019; Warchol, 2010), such as amikacin (Aksoy et al., 2015; Beaubien et al., 1989, 1990; Beaubien et al., 1991; Endo et al., 2022), gentamicin (Chatterton et al., 2022; Smyth et al., 2019), kanamycin (Brummett, Bendrick, & Himes, 1981; Ghafari et al., 2020; Mantefardo & Sisay, 2021; Voogt & Schoeman, 1996), neomycin (Kavanagh & McCabe, 1983; Ward & Rounthwaite, 1978) and streptomycin (Adeyemo, Oluwatosin, & Omotade, 2016; Md Daud, Mohamadl, Haron, & Rahman, 2014; Voogt & Schoeman, 1996; Wanamaker, Slepecky, Cefaratti, & Ogata, 1999).
Anti-microbial agents: Other anti-bacterial drugs
Beyond aminoglycosides (Buziashvili et al., 2019; Owusu, Amartey, Afutu, & Boafo, 2022; Stevenson, Biagio-de Jager, Graham, & Swanepoel, 2021), other agents used in the treatment of tuberculosis may also exhibit ototoxicity, such as isoniazid (Altiparmak, Pamuk, Pamuk, Ataman, & Serdengecti, 2002).
Some anti-bacterial agents from other classes also have documented ototoxicity, including the macrolide antibiotics erythromycin (Agusti, Ferran, Gea, & Picado, 1991; Bizjak, Haug, Schilz, Sarodia, & Dresing, 1999; Brummett, 1993; Levin & Behrenth, 1986; McGhan & Merchant, 2003; Moral et al., 1994; Sacristan et al., 1993; Schweitzer & Olson, 1984; Swanson et al., 1992; Thompson, Wood, & Bergstrom, 1980; van Marion, van der Meer, Kalff, & Schicht, 1978) and azithromycin (Haydon, Thelin, & Davis, 1984; Mamikoglu & Mamikoglu, 2001; Wallace, Miller, Nguyen, & Shields, 1994), and the glycopeptide antibiotic vancomycin (Gendeh, Gibb, Aziz, Kong, & Zahir, 1998; Gomceli, Vangala, Zeana, Kelly, & Singh, 2018; Humphrey, Veve, Walker, & Shorman, 2019; Kavanagh & McCabe, 1983; Lestner, Hill, Heath, & Sharland, 2016; Marissen et al., 2020; Mellor, Kingdom, Cafferkey, & Keane, 1984; Traber & Levine, 1981).
Anti-microbial agents: Anti-fungal drugs
Some anti-fungal agents, such as amphotericin (Ramu et al., 2021; Singh & Sharma, 2019), have documented ototoxicity.
Anti-microbial agents: Anti-parasitic drugs
Several anti-malarial medications have documented ototoxicity (Dillard, Fullerton, & McMahon, 2021; Jozefowicz-Korczynska, Pajor, & Lucas Grzelczyk, 2021).
Quinine and its derivatives
Quinine-based drugs are used as anti-malarial agents (Dillard et al., 2021; Jozefowicz-Korczynska et al., 2021) and against certain autoimmune diseases such as rheumatoid arthritis; some of these medications have documented ototoxicity. These include quinine itself (Nielsen-Abbring, Perenboom, & van der Hulst, 1990; Semedo, Dias-Silva, Migueis, & Pita, 2021; Tange, Dreschler, Claessen, & Perenboom, 1997), chloroquine (Bortoli & Santiago, 2007; Fernandes, Vernier, Dallegrave, & Machado, 2022) and hydroxychloroquine (Fernandes et al., 2022).
Anti-arrhythmic agents
Some anti-arrhythmic agents, such as amiodarone (Gurkov, 2018; Gurkov et al., 2017), have been reported to exhibit ototoxic properties.
Immunosuppressants
Several medications and medication classes that influence the immune system have documented ototoxicity. These include a variety of immunosuppressants (Franz et al., 2022) such as cyclosporine (Waissbluth, 2020).
Anti-neoplastic agents: Platinum derivatives
Platinum based anti-neoplastic agents have well-documented ototoxicity. The oldest of these medications, cisplatin, is perhaps the most ototoxic of these (Brock 2022; Hodge et al. 2021; Low et al. 2010; Nitz et al. 2013; Paken et al. 2016, 2019; Rybak et al. 2007; Sanchez et al. 2023; Santucci et al. 2021; Sriyapai et al. 2022; Tserga et al. 2019; Yildirim et al. 2022). Newer platinum-based agents are less so, but still ototoxic, including carboplatin (Batra et al. 2015; Bhagat et al. 2010; Cavaletti et al. 1998; Chevreau et al. 2005; Geurtsen et al. 2017; Kennedy et al. 1990; Musial-Bright et al. 2011; Nitz et al. 2013; Parsons et al. 1998; Qaddoumi et al. 2012; Waissbluth et al. 2018; Waissbluth et al. 2017) and oxaliplatin (Guvenc et al. 2016; Hijri et al. 2014; Malhotra et al. 2010; Oh et al. 2013; Vietor and George 2012).
Anti-neoplastic agents: Others
Other anti-neoplastic agents also have documented ototoxicity, including the taxane-derived anti-mitotic agent docetaxel (Xuan et al. 2020).
More recent anti-neoplastic agents, such as immune checkpoint inhibitors, have documented ototoxicity (Hu et al. 2020b; Lemasson et al. 2019; Sturmer et al. 2021).
Loop diuretics
Several loop diuretics have documented ototoxicity, including furosemide (Ahmed et al. 2012; Bates et al. 2002; Brummett et al. 1981; Halmagyi and Curthoys 2018; Kaka et al. 1984; Rybak 1985; Rybak and Whitworth 1986; Tuzel 1981) and bumetanide (Brummett et al. 1981; Tuzel 1981)
Other medications
Unregulated ototoxic medications (not requiring a prescription) include salicylates (Boettcher and Salvi 1991; Brien 1993; Day et al. 1989; Kim et al. 2013; Peleg et al. 2007; Stypulkowski 1990), the most common of which is acetylsalicylic acid (aspirin), which often is combined with other medications (such as in Excedrin Migraine).
Iron chelating agents have also documented ototoxicity (Derin et al. 2017).
Non-medical compounds
Various industrial volatile aromatic solvents (Fife et al. 2018; Gagnaire and Langlais 2005) have documented ototoxicity, such as styrene (Hoet and Lison 2008; Karasawa and Steyger 2015; Lawton et al. 2006; Makitie et al. 2003; Sass-Kortsak et al. 1995) and toluene (Hoet and Lison 2008; Juarez-Perez et al. 2014; Schaper et al. 2003; Schaper et al. 2008).
Various heavy metals have been implicated as ototoxic, including arsenic (Ishii et al. 2019; Kesici 2016; Kesici et al. 2016; Shokoohi et al. 2021) and mercury (Hoshino et al. 2012).
Marijuana may be ototoxic insofar as it can provoke tinnitus in some patients (Qian and Alyono 2020).
Natural history of ototoxicity
Generally ototoxicity is dose-dependent, so the larger the dose administered, and the more frequently the drug is administered, the more likely it is that ototoxic effects will occur, and the more pronounced those effects will be.
In contrast to the usual dose-dependent pattern are occasional case reports of dramatic toxicity from a single dose of medication (Garinis et al. 2021a; Gooi et al. 2008; Halmagyi and Curthoys 2018; Harruff et al. 2021; Yildirim et al. 2022).
Ototoxicity can be enhanced or potentiated by concomitant issues, such as renal insufficiency (which may impede excretion of the offending drug), co-administration with other agents (Aksoy et al. 2015; Bates et al. 2002; Brummett et al. 1981; Driessen et al. 2019; Kaka et al. 1984), specific genetic mutations(Clemens et al. 2020; Gao et al. 2017; McDermott et al. 2022; Nguyen and Jeyakumar 2019; Steyger 2021; Tserga et al. 2019; Turan et al. 2019), co-administration with radiation therapy (Cohen-Cutler et al. 2021; Driessen et al. 2019; Low et al. 2010; Low et al. 2020), ischemia (Lin et al. 2011) and noise exposure(Bhattacharyya and Dayal 1984; Brown et al. 1981; Castellanos and Fuente 2016; Garinis et al. 2021b; Li and Steyger 2009; Makitie et al. 2003; Steyger 2009). Whether these additional factors have a synergistic or merely additive effect is unclear.
Surprisingly, for some ototoxins there additionally appears to be a diurnal pattern of vulnerability (Blunston et al. 2015; Tserga et al. 2020).
Some longitudinal studies suggest that long-term hearing loss from cisplatin ototoxicity “dovetails” with age-related hearing loss (Skalleberg et al. 2021; Skalleberg et al. 2020).
Some studies describe some spontaneous improvement from vestibular ototoxicity in some vestibular testing parameters but not others (Black et al. 2001).
Can cochlear ototoxicity be monitored?
Since one of the most common ototoxic clinical manifestations is hearing loss, it is logical to look to assessment of hearing as a method for detecting and monitoring ototoxicity (Campbell and Durrant 1993; Le Prell et al. 2022; Simpson et al. 1992).
In ototoxicity from aminoglycoside antibiotics and platinum-based chemotherapeutic agents, usually cochleotoxicity initially affects high frequencies, and later affects low frequencies (Clemens et al. 2020; Gao et al. 2017; McDermott et al. 2022; Nguyen and Jeyakumar 2019; Steyger 2021; Tserga et al. 2019; Turan et al. 2019). Because of this pattern, methods for testing frequencies above those of a standard audiogram have been explored, including high-frequency audiometry (Caumo et al. 2017; Fausti et al. 1992, 1993; Fausti et al. 2003; Jacob et al. 2006; Singh Chauhan et al. 2011; van der Hulst et al. 1991) and otoacoustic emissions (Jacob et al. 2006).
Given the possibility of ototoxic agents directly affecting the cochlear nerve, some studies have explored the utility of using brainstem auditory evoked responses as a detection/monitoring technique (Bernard 1985; Chen et al. 2021; De Lauretis et al. 1999; Fausti et al. 1992, 1993; Ishii et al. 2019).
Beyond the idea of testing hearing, some studies have explored whether hearing tests can be performed with insert earphones (Gordon et al. 2005), whether they can be performed at home (Jacobs et al. 2012; Konrad-Martin et al. 2021) or even by a pharmacist (McKinzie et al. 2022) or by telehealth (Robler et al. 2022).
It has even been suggested that imaging the labyrinth by MRI (Veiga et al. 2021) or monitoring putative serum biomarkers (Generotti et al. 2022) might play a role in detecting/monitoring ototoxicity.
Despite various proposed monitoring recommendations (Bass and Bhagat 2014; Le Prell et al. 2022), no specific protocol has been widely adopted.
The clinical assessment of ototoxicity, and the broader scientific study of this subject, is sometimes complicated by medico-legal dimensions. An example of this is the legal practice (https://ksdlaw.com) of Keith S. Douglass (https://www.linkedin.com/in/keith-s-douglass-assoc-llp/) which focuses on medical malpractice claims related to aminoglycoside antibiotics.
Can vestibular ototoxicity be monitored?
The vast majority of ototoxicity literature pertains to cochleotoxicity.
Regrettably, the literature regarding vestibular ototoxicity is much more limited (Baguley and Prayuenyong 2020; Black et al. 2004; Black and Pesznecker 1993; Chatterton et al. 2022; Fife et al. 2018; Hsu et al. 2015; Jiang et al. 2021; Mount et al. 1995; Rutka 2019; Sedo-Cabezon et al. 2014; Smyth et al. 2019; Tsuji et al. 2000).
Can ototoxicity be prevented?
In many instances the use of an ototoxic medication is unavoidable, such in the chronic management of cystic fibrosis (Caumo et al. 2017; Dong et al. 2021; Elson et al. 2021; Garinis et al. 2021a; Harruff et al. 2021), or when a severe infection is only susceptible to an aminoglycoside antibiotic, or when an aggressive malignancy only responds to a platinum-based anti-neoplastic agent. Faced with likely ototoxicity in such circumstances, investigators have explored whether there are any mechanisms to attenuate ototoxicity (Barbara et al. 2022; Jiang et al. 2021; Laurell 2019; Pham et al. 2020; Rybak and Kelly 2003; Wu et al. 2021; Yurtsever et al. 2020; Zhang and Yu 2019; Zheng et al. 2020b).
Much of this research has been directed at aminoglycoside antibiotics (Kawamoto et al. 2004; Kitcher et al. 2019; Lopez-Gonzalez et al. 2000b; Momiyama et al. 2006; Pavlidis et al. 2014; Perletti et al. 2008; Zong et al. 2021), specifically at gentamicin (Kucharava et al. 2019; Niu et al. 2021; Wen et al. 2022), amikacin (Zadrozniak et al. 2019) and neomycin (Zheng et al. 2020a).
Considerable research has also explored otoprotective strategies against cisplatin ototoxicity (Bhatta et al. 2019; Drogemoller et al. 2019; Fang and Xiao 2014; Fernandez et al. 2021; Freyer et al. 2019; Freyer et al. 2020; Fritzsche et al. 2022; Guan et al. 2020; Hu et al. 2020a; Karasawa and Steyger 2015; Kitcher et al. 2019; Lee et al. 2020; Liang et al. 2021; Liu et al. 2021; Lopez-Gonzalez et al. 2000a; Navarro-Ruiz 2020; Paciello et al. 2020; Ruhl et al. 2019; Rybak et al. 2007; Santos et al. 2020; Simsek et al. 2019; Tan et al. 2022; Tas et al. 2021; Terzi et al. 2021; Wang et al. 2022; Wen et al. 2021; Yurtsever et al. 2020; Zhang et al. 2020; Zhang et al. 2022).
Relatively little research has been directed against ototoxicity from furosemide (Zadrozniak et al. 2019) and other agents.
Can ototoxicity be treated?
The short answer is that there is not yet any known direct therapy for any form of ototoxicity.
Hearing loss is usually treated with amplification by hearing aids, or (in severe cases) with cochlear implantation.
Imbalance is usually treated with vestibular rehabilitation therapy.
References
Adeyemo AA, Oluwatosin O, Omotade OO (2016) Study of streptomycin-induced ototoxicity: protocol for a longitudinal study. Springerplus 5: 758. doi: 10.1186/s40064-016-2429-5
Agusti C, Ferran F, Gea J, Picado C (1991) Ototoxic reaction to erythromycin. Arch Intern Med 151: 380. doi: 10.1001/archinte.1991.00400020124025
Ahmed RM, Hannigan IP, MacDougall HG, Chan RC, Halmagyi GM (2012) Gentamicin ototoxicity: a 23-year selected case series of 103 patients. Med J Aust 196: 701-4.
Aksoy F, Dogan R, Ozturan O, Yildirim YS, Veyseller B, Yenigun A, Ozturk B (2015) Betahistine exacerbates amikacin ototoxicity. Ann Otol Rhinol Laryngol 124: 280-7. doi: 10.1177/0003489414557020
Altiparmak MR, Pamuk ON, Pamuk GE, Ataman R, Serdengecti K (2002) Is isoniazid ototoxic in patients undergoing hemodialysis? Nephron 92: 478-80. doi: 10.1159/000063306
Baguley DM, Prayuenyong P (2020) Looking beyond the audiogram in ototoxicity associated with platinum-based chemotherapy. Cancer Chemother Pharmacol 85: 245-250. doi: 10.1007/s00280-019-04012-z
Barbara M, Margani V, Covelli E, Filippi C, Volpini L, El-Borady OM, El-Kemary M, Elzayat S, Elfarargy HH (2022) The Use of Nanoparticles in Otoprotection. Front Neurol 13: 912647. doi: 10.3389/fneur.2022.912647
Bass JK, Bhagat SP (2014) Challenges in ototoxicity monitoring in the pediatric oncology population. J Am Acad Audiol 25: 760-74; quiz 782-3. doi: 10.3766/jaaa.25.8.6
Bates DE, Beaumont SJ, Baylis BW (2002) Ototoxicity induced by gentamicin and furosemide. Ann Pharmacother 36: 446-51. doi: 10.1345/aph.1A216
Batra A, Thakar A, Bakhshi S (2015) Ototoxicity in retinoblastoma survivors treated with carboplatin based chemotherapy: A cross-sectional study of 116 patients. Pediatr Blood Cancer 62: 2060. doi: 10.1002/pbc.25618
Beaubien AR, Desjardins S, Ormsby E, Bayne A, Carrier K, Cauchy MJ, Henri R, Hodgen M, Salley J, St Pierre A (1989) Incidence of amikacin ototoxicity: a sigmoid function of total drug exposure independent of plasma levels. Am J Otolaryngol 10: 234-43. doi: 10.1016/0196-0709(89)90002-1
Beaubien AR, Desjardins S, Ormsby E, Bayne A, Carrier K, Cauchy MJ, Henri R, Hodgen M, Salley J, St Pierre A (1990) Delay in hearing loss following drug administration. A consistent feature of amikacin ototoxicity. Acta Otolaryngol 109: 345-52. doi: 10.3109/00016489009125154
Beaubien AR, Ormsby E, Bayne A, Carrier K, Crossfield G, Downes M, Henri R, Hodgen M (1991) Evidence that amikacin ototoxicity is related to total perilymph area under the concentration-time curve regardless of concentration. Antimicrob Agents Chemother 35: 1070-4. doi: 10.1128/AAC.35.6.1070
Bernard P (1985) Alterations of auditory evoked potentials during the course of chloroquine treatment. Acta Otolaryngol 99: 387-92. doi: 10.3109/00016488509108928
Bhagat SP, Bass JK, White ST, Qaddoumi I, Wilson MW, Wu J, Rodriguez-Galindo C (2010) Monitoring carboplatin ototoxicity with distortion-product otoacoustic emissions in children with retinoblastoma. Int J Pediatr Otorhinolaryngol 74: 1156-63. doi: 10.1016/j.ijporl.2010.07.004
Bhatta P, Dhukhwa A, Sheehan K, Al Aameri RFH, Borse V, Ghosh S, Sheth S, Mamillapalli C, Rybak L, Ramkumar V, Mukherjea D (2019) Capsaicin Protects Against Cisplatin Ototoxicity by Changing the STAT3/STAT1 Ratio and Activating Cannabinoid (CB2) Receptors in the Cochlea. Sci Rep 9: 4131. doi: 10.1038/s41598-019-40425-9
Bhattacharyya TK, Dayal VS (1984) Ototoxicity and noise-drug interaction. J Otolaryngol 13: 361-6.
Bizjak ED, Haug MT, 3rd, Schilz RJ, Sarodia BD, Dresing JM (1999) Intravenous azithromycin-induced ototoxicity. Pharmacotherapy 19: 245-8. doi: 10.1592/phco.19.3.245.30930
Black FO, Gianna-Poulin C, Pesznecker SC (2001) Recovery from vestibular ototoxicity. Otol Neurotol 22: 662-71. doi: 10.1097/00129492-200109000-00018
Black FO, Pesznecker S, Stallings V (2004) Permanent gentamicin vestibulotoxicity. Otol Neurotol 25: 559-69. doi: 10.1097/00129492-200407000-00025
Black FO, Pesznecker SC (1993) Vestibular ototoxicity. Clinical considerations. Otolaryngol Clin North Am 26: 713-36.
Blunston MA, Yonovitz A, Woodahl EL, Smolensky MH (2015) Gentamicin-induced ototoxicity and nephrotoxicity vary with circadian time of treatment and entail separate mechanisms. Chronobiol Int 32: 1223-32. doi: 10.3109/07420528.2015.1082483
Boettcher FA, Salvi RJ (1991) Salicylate ototoxicity: review and synthesis. Am J Otolaryngol 12: 33-47. doi: 10.1016/0196-0709(91)90071-m
Bortoli R, Santiago M (2007) Chloroquine ototoxicity. Clin Rheumatol 26: 1809-10. doi: 10.1007/s10067-007-0662-6
Brien JA (1993) Ototoxicity associated with salicylates. A brief review. Drug Saf 9: 143-8. doi: 10.2165/00002018-199309020-00006
Brock PR (2022) New insights into cisplatin ototoxicity. Cancer 128: 43-46. doi: 10.1002/cncr.33847
Brown RD, Penny JE, Henley CM, Hodges KB, Kupetz SA, Glenn DW, Jobe JC (1981) Ototoxic drugs and noise. Ciba Found Symp 85: 151-71. doi: 10.1002/9780470720677.ch9
Brummett RE (1993) Ototoxic liability of erythromycin and analogues. Otolaryngol Clin North Am 26: 811-9.
Brummett RE, Bendrick T, Himes D (1981) Comparative ototoxicity of bumetanide and furosemide when used in combination with kanamycin. J Clin Pharmacol 21: 628-36. doi: 10.1002/j.1552-4604.1981.tb05675.x
Buziashvili M, Mirtskhulava V, Kipiani M, Blumberg HM, Baliashvili D, Magee MJ, Furin JJ, Tukvadze N, Kempker RR (2019) Rates and risk factors for nephrotoxicity and ototoxicity among tuberculosis patients in Tbilisi, Georgia. Int J Tuberc Lung Dis 23: 1005-1011. doi: 10.5588/ijtld.18.0626
Campbell KC, Durrant J (1993) Audiologic monitoring for ototoxicity. Otolaryngol Clin North Am 26: 903-14.
Castellanos MJ, Fuente A (2016) The Adverse Effects of Heavy Metals with and without Noise Exposure on the Human Peripheral and Central Auditory System: A Literature Review. Int J Environ Res Public Health 13. doi: 10.3390/ijerph13121223
Caumo DTM, Geyer LB, Teixeira AR, Barreto SSM (2017) Hearing thresholds at high frequency in patients with cystic fibrosis: a systematic review. Braz J Otorhinolaryngol 83: 464-474. doi: 10.1016/j.bjorl.2016.10.006
Cavaletti G, Bogliun G, Zincone A, Marzorati L, Melzi P, Frattola L, Marzola M, Bonazzi C, Cantu MG, Chiari S, Galli A, Bregni M, Gianni MA (1998) Neuro- and ototoxicity of high-dose carboplatin treatment in poor prognosis ovarian cancer patients. Anticancer Res 18: 3797-802.
Chatterton S, Wang C, Satyan H, Kotsiou G, Todd CJ, Migliaccio AA, Cremer PD (2022) A Prospective Study on the Vestibular Toxicity of Gentamicin in a Clinical Setting. Otol Neurotol 43: e1029-e1033. doi: 10.1097/MAO.0000000000003663
Chen Y, Bielefeld EC, Mellott JG, Wang W, Mafi AM, Yamoah EN, Bao J (2021) Early Physiological and Cellular Indicators of Cisplatin-Induced Ototoxicity. J Assoc Res Otolaryngol 22: 107-126. doi: 10.1007/s10162-020-00782-z
Chevreau C, Thomas F, Couteau C, Dalenc F, Mourey L, Chatelut E (2005) Ototoxicity of high-dose carboplatin. J Clin Oncol 23: 3649-50; author reply 3650-1. doi: 10.1200/JCO.2005.05.348
Clemens E, Broer L, Langer T, Uitterlinden AG, de Vries ACH, van Grotel M, Pluijm SFM, Binder H, Byrne J, Broeder EVD, Crocco M, Grabow D, Kaatsch P, Kaiser M, Kenborg L, Winther JF, Rechnitzer C, Hasle H, Kepak T, van der Kooi AF, Kremer LC, Kruseova J, Kuehni CE, van der Pal H, Parfitt R, Deuster D, Matulat P, Spix C, Tillmanns A, Tissing WJE, Maier L, Am Zehnhoff-Dinnesen A, Zolk O, van den Heuvel-Eibrink MM, PanCare Lc (2020) Genetic variation of cisplatin-induced ototoxicity in non-cranial-irradiated pediatric patients using a candidate gene approach: The International PanCareLIFE Study. Pharmacogenomics J 20: 294-305. doi: 10.1038/s41397-019-0113-1
Cohen-Cutler S, Wong K, Mena V, Sianto K, Wright MA, Olch A, Orgel E (2021) Hearing Loss Risk in Pediatric Patients Treated with Cranial Irradiation and Cisplatin-Based Chemotherapy. Int J Radiat Oncol Biol Phys 110: 1488-1495. doi: 10.1016/j.ijrobp.2021.02.050
Day RO, Graham GG, Bieri D, Brown M, Cairns D, Harris G, Hounsell J, Platt-Hepworth S, Reeve R, Sambrook PN, et al. (1989) Concentration-response relationships for salicylate-induced ototoxicity in normal volunteers. Br J Clin Pharmacol 28: 695-702. doi: 10.1111/j.1365-2125.1989.tb03562.x
De Lauretis A, De Capua B, Barbieri MT, Bellussi L, Passali D (1999) ABR evaluation of ototoxicity in cancer patients receiving cisplatin or carboplatin. Scand Audiol 28: 139-43. doi: 10.1080/010503999424707
Derin S, Azik FM, Topal Y, Topal H, Karakus V, Cetinkaya PU, Sahan M, Azik TE, Kocabas CN (2017) The Incidence of Ototoxicity in Patients Using Iron Chelators. J Int Adv Otol 13: 136-139. doi: 10.5152/iao.2016.1852
Dillard LK, Fullerton AM, McMahon CM (2021) Ototoxic hearing loss from antimalarials: A systematic narrative review. Travel Med Infect Dis 43: 102117. doi: 10.1016/j.tmaid.2021.102117
Dong M, Rodriguez AV, Blankenship CA, McPhail G, Vinks AA, Hunter LL (2021) Pharmacokinetic modelling to predict risk of ototoxicity with intravenous tobramycin treatment in cystic fibrosis. J Antimicrob Chemother 76: 2923-2931. doi: 10.1093/jac/dkab288
Driessen CML, Leijendeckers J, Snik A, van der Graaf WTA, de Boer JP, Gelderblom H, Kaanders J, Takes R, van Herpen CML (2019) Ototoxicity in locally advanced head and neck cancer patients treated with induction chemotherapy followed by intermediate or high-dose cisplatin-based chemoradiotherapy. Head Neck 41: 488-494. doi: 10.1002/hed.25434
Drogemoller BI, Wright GEB, Lo C, Le T, Brooks B, Bhavsar AP, Rassekh SR, Ross CJD, Carleton BC (2019) Pharmacogenomics of Cisplatin-Induced Ototoxicity: Successes, Shortcomings, and Future Avenues of Research. Clin Pharmacol Ther 106: 350-359. doi: 10.1002/cpt.1483
Elson EC, Meier E, Oermann CM (2021) The implementation of an aminoglycoside induced ototoxicity algorithm for people with cystic fibrosis. J Cyst Fibros 20: 284-287. doi: 10.1016/j.jcf.2020.08.002
Endo A, Hanawa K, Nemoto A, Ishikawa T, Kazama S, Kagami Y, Maebayashi Y, Katsumata N, Naito A, Kobayashi Y, Kawano Y, Hanawa T (2022) Evaluation of nephrotoxicity and ototoxicity following amikacin administration once daily or every 48 hours in neonates. Medicine (Baltimore) 101: e31425. doi: 10.1097/MD.0000000000031425
Fang B, Xiao H (2014) Rapamycin alleviates cisplatin-induced ototoxicity in vivo. Biochem Biophys Res Commun 448: 443-7. doi: 10.1016/j.bbrc.2014.04.123
Fausti SA, Frey RH, Henry JA, Olson DJ, Schaffer HI (1992) Early detection of ototoxicity using high-frequency, tone-burst-evoked auditory brainstem responses. J Am Acad Audiol 3: 397-404.
Fausti SA, Frey RH, Henry JA, Olson DJ, Schaffer HI (1993) High-frequency testing techniques and instrumentation for early detection of ototoxicity. J Rehabil Res Dev 30: 333-41.
Fausti SA, Helt WJ, Phillips DS, Gordon JS, Bratt GW, Sugiura KM, Noffsinger D (2003) Early detection of ototoxicity using 1/6th-octave steps. J Am Acad Audiol 14: 444-50.
Fernandes CP, Vernier LS, Dallegrave E, Machado MS (2022) The Ototoxicity of Chloroquine and Hydroxychloroquine: A Systematic Review. Int Arch Otorhinolaryngol 26: e167-e177. doi: 10.1055/s-0041-1740986
Fernandez KA, Allen P, Campbell M, Page B, Townes T, Li CM, Cheng H, Garrett J, Mulquin M, Clements A, Mulford D, Ortiz C, Brewer C, Dubno JR, Newlands S, Schmitt NC, Cunningham LL (2021) Atorvastatin is associated with reduced cisplatin-induced hearing loss. J Clin Invest 131. doi: 10.1172/JCI142616
Fife TD, Robb MJA, Steenerson KK, Saha KC (2018) Bilateral Vestibular Dysfunction Associated With Chronic Exposure to Military Jet Propellant Type-Eight Jet Fuel. Front Neurol 9: 351. doi: 10.3389/fneur.2018.00351
Franz L, Frosolini A, Parrino D, Lovato A, de Filippis C, Marioni G (2022) Ototoxicity of Immunosuppressant Drugs: A Systematic Review. J Int Adv Otol 18: 167-176. doi: 10.5152/iao.2022.21416
Freyer DR, Brock P, Knight K, Reaman G, Cabral S, Robinson PD, Sung L (2019) Interventions for cisplatin-induced hearing loss in children and adolescents with cancer. Lancet Child Adolesc Health 3: 578-584. doi: 10.1016/S2352-4642(19)30115-4
Freyer DR, Brock PR, Chang KW, Dupuis LL, Epelman S, Knight K, Mills D, Phillips R, Potter E, Risby D, Simpkin P, Sullivan M, Cabral S, Robinson PD, Sung L (2020) Prevention of cisplatin-induced ototoxicity in children and adolescents with cancer: a clinical practice guideline. Lancet Child Adolesc Health 4: 141-150. doi: 10.1016/S2352-4642(19)30336-0
Fritzsche S, Strauss C, Scheller C, Leisz S (2022) Nimodipine Treatment Protects Auditory Hair Cells from Cisplatin-Induced Cell Death Accompanied by Upregulation of LMO4. Int J Mol Sci 23. doi: 10.3390/ijms23105780
Gagnaire F, Langlais C (2005) Relative ototoxicity of 21 aromatic solvents. Arch Toxicol 79: 346-54. doi: 10.1007/s00204-004-0636-2
Gao Z, Chen Y, Guan MX (2017) Mitochondrial DNA mutations associated with aminoglycoside induced ototoxicity. J Otol 12: 1-8. doi: 10.1016/j.joto.2017.02.001
Garinis A, Gleser M, Johns A, Larsen E, Vachhani J (2021a) Prospective cohort study of ototoxicity in persons with cystic fibrosis following a single course of intravenous tobramycin. J Cyst Fibros 20: 278-283. doi: 10.1016/j.jcf.2020.07.001
Garinis A, Konrad-Martin D, Bramhall N (2021b) Ototoxicity and Noise Damage: From Preclinical Findings to Audiological Management. Am J Audiol 30: 797-799. doi: 10.1044/2021_AJA-21-00153
Gendeh BS, Gibb AG, Aziz NS, Kong N, Zahir ZM (1998) Vancomycin administration in continuous ambulatory peritoneal dialysis: the risk of ototoxicity. Otolaryngol Head Neck Surg 118: 551-8. doi: 10.1177/019459989811800420
Generotti C, Cox BC, Singh J, Hamilton D, McKenzie E, O’Malley BW, Jr., Li D (2022) Subclinical diagnosis of cisplatin-induced ototoxicity with biomarkers. Sci Rep 12: 18032. doi: 10.1038/s41598-022-23034-x
Geurtsen ML, Kors WA, Moll AC, Smits C (2017) Long-term audiologic follow-up of carboplatin-treated children with retinoblastoma. Ophthalmic Genet 38: 74-78. doi: 10.3109/13816810.2015.1137325
Ghafari N, Court R, Chirehwa MT, Wiesner L, Petersen L, Maartens G, Gumbo T, McIlleron H, Ramma L (2020) Pharmacokinetics and other risk factors for kanamycin-induced hearing loss in patients with multi-drug resistant tuberculosis. Int J Audiol 59: 219-223. doi: 10.1080/14992027.2019.1690170
Gomceli U, Vangala S, Zeana C, Kelly PJ, Singh M (2018) An Unusual Case of Ototoxicity with Use of Oral Vancomycin. Case Rep Infect Dis 2018: 2980913. doi: 10.1155/2018/2980913
Gooi A, Hochman J, Wellman M, Blakley L, Blakley BW (2008) Ototoxic effects of single-dose versus 19-day daily-dose gentamicin. J Otolaryngol Head Neck Surg 37: 664-7.
Gordon JS, Phillips DS, Helt WJ, Konrad-Martin D, Fausti SA (2005) Evaluation of insert earphones for high-frequency bedside ototoxicity monitoring. J Rehabil Res Dev 42: 353-61. doi: 10.1682/jrrd.2004.06.0093
Guan G, He X, Chen J, Bin L, Tang X (2020) Identifying the mechanisms underlying the protective effect of tetramethylpyrazine against cisplatin‑induced in vitro ototoxicity in HEI‑OC1 auditory cells using gene expression profiling. Mol Med Rep 22: 5053-5068. doi: 10.3892/mmr.2020.11631
Gurkov R (2018) Amiodarone: A Newly Discovered Association with Bilateral Vestibulopathy. Front Neurol 9: 119. doi: 10.3389/fneur.2018.00119
Gurkov R, Manzari L, Blodow A, Wenzel A, Pavlovic D, Luis L (2017) Amiodarone-associated bilateral vestibulopathy. Eur Arch Otorhinolaryngol. doi: 10.1007/s00405-017-4858-3
Guvenc MG, Dizdar D, Dizdar SK, Okutur SK, Demir G (2016) Sudden hearing loss due to oxaliplatin use in a patient with colon cancer. J Chemother 28: 341-2. doi: 10.1179/1973947815Y.0000000023
Halmagyi GM, Curthoys IS (2018) Adverse effects of a single dose of gentamicin. Br J Clin Pharmacol. doi: 10.1111/bcp.13667
Harruff EE, Kil J, Ortiz MGT, Dorgan D, Jain R, Poth EA, Fifer RC, Kim YJM, Shoup AG, Flume PA (2021) Ototoxicity in cystic fibrosis patients receiving intravenous tobramycin for acute pulmonary exacerbation: Ototoxicity following tobramycin treatment. J Cyst Fibros 20: 288-294. doi: 10.1016/j.jcf.2020.11.020
Haydon RC, Thelin JW, Davis WE (1984) Erythromycin ototoxicity: analysis and conclusions based on 22 case reports. Otolaryngol Head Neck Surg 92: 678-84. doi: 10.1177/019459988409200615
Henley CM, 3rd, Schacht J (1988) Pharmacokinetics of aminoglycoside antibiotics in blood, inner-ear fluids and tissues and their relationship to ototoxicity. Audiology 27: 137-46. doi: 10.3109/00206098809081584
Hijri FZ, Arifi S, Ouattassi N, Mellas N, El Mesbahi O (2014) Oxaliplatin-induced ototoxicity in adjuvant setting for colorectal cancer: unusual side effect. J Gastrointest Cancer 45: 106-8. doi: 10.1007/s12029-013-9489-3
Hodge SE, Lopez IA, Ishiyama G, Ishiyama A (2021) Cisplatin ototoxicity histopathology. Laryngoscope Investig Otolaryngol 6: 852-856. doi: 10.1002/lio2.608
Hoet P, Lison D (2008) Ototoxicity of toluene and styrene: state of current knowledge. Crit Rev Toxicol 38: 127-70. doi: 10.1080/10408440701845443
Hoshino AC, Ferreira HP, Malm O, Carvallo RM, Camara VM (2012) A systematic review of mercury ototoxicity. Cad Saude Publica 28: 1239-48. doi: 10.1590/s0102-311×2012000700003
Hsu PC, Cheng PW, Young YH (2015) Ototoxicity from organic solvents assessed by an inner ear test battery. J Vestib Res 25: 177-83. doi: 10.3233/VES-150559
Hu B, Liu Y, Chen X, Zhao J, Han J, Dong H, Zheng Q, Nie G (2020a) Ferrostatin-1 protects auditory hair cells from cisplatin-induced ototoxicity in vitro and in vivo. Biochem Biophys Res Commun 533: 1442-1448. doi: 10.1016/j.bbrc.2020.10.019
Hu F, Ye X, Zhai Y, Xu J, Guo X, Guo Z, Zhou X, Ruan Y, Zhuang Y, He J (2020b) Ear and labyrinth toxicities induced by immune checkpoint inhibitors: a disproportionality analysis from 2014 to 2019. Immunotherapy 12: 531-540. doi: 10.2217/imt-2019-0120
Humphrey C, Veve MP, Walker B, Shorman MA (2019) Long-term vancomycin use had low risk of ototoxicity. PLoS One 14: e0224561. doi: 10.1371/journal.pone.0224561
Huth ME, Ricci AJ, Cheng AG (2011) Mechanisms of aminoglycoside ototoxicity and targets of hair cell protection. Int J Otolaryngol 2011: 937861. doi: 10.1155/2011/937861
Ishii N, Mochizuki H, Yamashita M, Yagi K, Shiomi K, Tsuruta K, Nakazato M (2019) Auditory brainstem response analysis for long-term central auditory function sequelae in patients with chronic arsenic intoxication: A cross-sectional study. J Neurol Sci 398: 2-3. doi: 10.1016/j.jns.2019.01.010
Jacob LC, Aguiar FP, Tomiasi AA, Tschoeke SN, Bitencourt RF (2006) Auditory monitoring in ototoxicity. Braz J Otorhinolaryngol 72: 836-44. doi: 10.1016/s1808-8694(15)31053-3
Jacobs PG, Silaski G, Wilmington D, Gordon S, Helt W, McMillan G, Fausti SA, Dille M (2012) Development and evaluation of a portable audiometer for high-frequency screening of hearing loss from ototoxicity in homes/clinics. IEEE Trans Biomed Eng 59: 3097-103. doi: 10.1109/TBME.2012.2204881
Jiang L, Zheng Z, He Y (2021) Progress in protecting vestibular hair cells. Arch Toxicol 95: 2613-2623. doi: 10.1007/s00204-021-03067-3
Jozefowicz-Korczynska M, Pajor A, Lucas Grzelczyk W (2021) The Ototoxicity of Antimalarial Drugs-A State of the Art Review. Front Neurol 12: 661740. doi: 10.3389/fneur.2021.661740
Juarez-Perez CA, Torres-Valenzuela A, Haro-Garcia LC, Borja-Aburto VH, Aguilar-Madrid G (2014) Ototoxicity effects of low exposure to solvent mixture among paint manufacturing workers. Int J Audiol 53: 370-6. doi: 10.3109/14992027.2014.888597
Kaka JS, Lyman C, Kilarski DJ (1984) Tobramycin-furosemide interaction. Drug Intell Clin Pharm 18: 235-8. doi: 10.1177/106002808401800310
Karasawa T, Steyger PS (2015) An integrated view of cisplatin-induced nephrotoxicity and ototoxicity. Toxicol Lett 237: 219-27. doi: 10.1016/j.toxlet.2015.06.012
Kavanagh KT, McCabe BF (1983) Ototoxicity of oral neomycin and vancomycin. Laryngoscope 93: 649-53. doi: 10.1002/lary.1983.93.5.649
Kawamoto K, Sha SH, Minoda R, Izumikawa M, Kuriyama H, Schacht J, Raphael Y (2004) Antioxidant gene therapy can protect hearing and hair cells from ototoxicity. Mol Ther 9: 173-81. doi: 10.1016/j.ymthe.2003.11.020
Kennedy IC, Fitzharris BM, Colls BM, Atkinson CH (1990) Carboplatin is ototoxic. Cancer Chemother Pharmacol 26: 232-4. doi: 10.1007/BF02897206
Kesici GG (2016) Arsenic ototoxicity. J Otol 11: 13-17. doi: 10.1016/j.joto.2016.03.001
Kesici GG, Unlu I, Topcu AB, Bal CD, Tutkun E, Yilmaz OH (2016) Arsenic related hearing loss in miners. Am J Otolaryngol 37: 6-11. doi: 10.1016/j.amjoto.2015.09.003
Kim SM, Jo JM, Baek MJ, Jung KH (2013) A case of bilateral sudden hearing loss and tinnitus after salicylate intoxication. Korean J Audiol 17: 23-6. doi: 10.7874/kja.2013.17.1.23
Kitcher SR, Kirkwood NK, Camci ED, Wu P, Gibson RM, Redila VA, Simon JA, Rubel EW, Raible DW, Richardson GP, Kros CJ (2019) ORC-13661 protects sensory hair cells from aminoglycoside and cisplatin ototoxicity. JCI Insight 4. doi: 10.1172/jci.insight.126764
Konrad-Martin D, O’Connell Bennett K, Garinis A, McMillan GP (2021) A Randomized Controlled Trial Using Automated Technology for Improving Ototoxicity Monitoring in VA Oncology Patients. Am J Audiol 30: 870-886. doi: 10.1044/2021_AJA-21-00032
Kucharava K, Sekulic-Jablanovic M, Horvath L, Bodmer D, Petkovic V (2019) Pasireotide protects mammalian cochlear hair cells from gentamicin ototoxicity by activating the PI3K-Akt pathway. Cell Death Dis 10: 110. doi: 10.1038/s41419-019-1386-7
Laurell G (2019) Pharmacological intervention in the field of ototoxicity. HNO 67: 434-439. doi: 10.1007/s00106-019-0663-1
Lawton BW, Hoffmann J, Triebig G (2006) The ototoxicity of styrene: a review of occupational investigations. Int Arch Occup Environ Health 79: 93-102. doi: 10.1007/s00420-005-0030-2
Le Prell CG, Brewer CC, Campbell KCM (2022) The audiogram: Detection of pure-tone stimuli in ototoxicity monitoring and assessments of investigational medicines for the inner ear. J Acoust Soc Am 152: 470. doi: 10.1121/10.0011739
Lee CH, Lee DH, Lee SM, Kim ASY (2020) Otoprotective Effects of Zingerone on Cisplatin-Induced Ototoxicity. Int J Mol Sci 21. doi: 10.3390/ijms21103503
Lemasson J, Cuzzubbo S, Doucet L, Gounant V, Baroudjian B, Herms F, Carpentier AF, Lebbe C, Vitaux H, Hautefort C, Delyon J, group P (2019) Cochleovestibular toxicity induced by immune checkpoint inhibition: a case series. Eur J Cancer 117: 116-118. doi: 10.1016/j.ejca.2019.05.022
Lestner JM, Hill LF, Heath PT, Sharland M (2016) Vancomycin toxicity in neonates: a review of the evidence. Curr Opin Infect Dis 29: 237-47. doi: 10.1097/QCO.0000000000000263
Levin G, Behrenth E (1986) Irreversible ototoxic effect of erythromycin. Scand Audiol 15: 41-2. doi: 10.3109/01050398609045952
Li H, Steyger PS (2009) Synergistic ototoxicity due to noise exposure and aminoglycoside antibiotics. Noise Health 11: 26-32. doi: 10.4103/1463-1741.45310
Liang Z, Zhang T, Zhan T, Cheng G, Zhang W, Jia H, Yang H (2021) Metformin alleviates cisplatin-induced ototoxicity by autophagy induction possibly via the AMPK/FOXO3a pathway. J Neurophysiol 125: 1202-1212. doi: 10.1152/jn.00417.2020
Lin CD, Kao MC, Tsai MH, Lai CH, Wei IH, Tsai MH, Tang CH, Lin CW, Hsu CJ, Lin CY (2011) Transient ischemia/hypoxia enhances gentamicin ototoxicity via caspase-dependent cell death pathway. Lab Invest 91: 1092-106. doi: 10.1038/labinvest.2011.69
Liu Y, Wu H, Zhang F, Yang J, He J (2021) Resveratrol upregulates miR-455-5p to antagonize cisplatin ototoxicity via modulating the PTEN-PI3K-AKT axis. Biochem Cell Biol 99: 385-395. doi: 10.1139/bcb-2020-0459
Lopez-Gonzalez MA, Guerrero JM, Rojas F, Delgado F (2000a) Ototoxicity caused by cisplatin is ameliorated by melatonin and other antioxidants. J Pineal Res 28: 73-80. doi: 10.1034/j.1600-079x.2001.280202.x
Lopez-Gonzalez MA, Guerrero JM, Torronteras R, Osuna C, Delgado F (2000b) Ototoxicity caused by aminoglycosides is ameliorated by melatonin without interfering with the antibiotic capacity of the drugs. J Pineal Res 28: 26-33. doi: 10.1034/j.1600-079x.2000.280104.x
Low WK, Kong SW, Tan MG (2010) Ototoxicity from combined Cisplatin and radiation treatment: an in vitro study. Int J Otolaryngol 2010: 523976. doi: 10.1155/2010/523976
Low WK, Teng SW, Tan MGK (2020) Synergistic Ototoxicity of Gentamicin and Low-Dose Irradiation: Molecular Basis and Clinical Significance. Audiol Neurootol 25: 111-119. doi: 10.1159/000503133
Makitie AA, Pirvola U, Pyykko I, Sakakibara H, Riihimaki V, Ylikoski J (2003) The ototoxic interaction of styrene and noise. Hear Res 179: 9-20. doi: 10.1016/s0378-5955(03)00066-2
Malhotra NK, Aslam R, Lipman SP, Bilski VJ (2010) Acute ototoxicity from a single infusion of oxaliplatin. Ear Nose Throat J 89: 258-61.
Mamikoglu B, Mamikoglu O (2001) Irreversible sensorineural hearing loss as a result of azithromycin ototoxicity. A case report. Ann Otol Rhinol Laryngol 110: 102. doi: 10.1177/000348940111000119
Mantefardo B, Sisay G (2021) Case Report: Kanamycin Ototoxicity and MDR-TB Treatment Regimen. Int Med Case Rep J 14: 815-817. doi: 10.2147/IMCRJ.S336259
Marissen J, Fortmann I, Humberg A, Rausch TK, Simon A, Stein A, Schaible T, Eichhorn J, Wintgens J, Roll C, Heitmann F, Herting E, Gopel W, Hartel C (2020) Vancomycin-induced ototoxicity in very-low-birthweight infants. J Antimicrob Chemother 75: 2291-2298. doi: 10.1093/jac/dkaa156
McDermott JH, Mahaveer A, James RA, Booth N, Turner M, Harvey KE, Miele G, Beaman GM, Stoddard DC, Tricker K, Corry RJ, Garlick J, Ainsworth S, Beevers T, Bruce IA, Body R, Ulph F, MacLeod R, Roberts PL, Wilson PM, Newman WG, Team PS (2022) Rapid Point-of-Care Genotyping to Avoid Aminoglycoside-Induced Ototoxicity in Neonatal Intensive Care. JAMA Pediatr 176: 486-492. doi: 10.1001/jamapediatrics.2022.0187
McGhan LJ, Merchant SN (2003) Erythromycin ototoxicity. Otol Neurotol 24: 701-2. doi: 10.1097/00129492-200307000-00029
McKinzie CJ, Kam CW, Parry R, Darby M, Tak CR (2022) Pharmacist-administered audiology screening for pediatric cystic fibrosis patients exposed to high-dose aminoglycosides: A pilot study. Pediatr Pulmonol 57: 1814-1817. doi: 10.1002/ppul.25946
Md Daud MK, Mohamadl H, Haron A, Rahman NA (2014) Ototoxicity screening of patients treated with streptomycin using distortion product otoacoustic emissions. B-ENT 10: 53-8.
Mellor JA, Kingdom J, Cafferkey M, Keane C (1984) Vancomycin ototoxicity in patients with normal renal function. Br J Audiol 18: 179-80. doi: 10.3109/03005368409078946
Momiyama J, Hashimoto T, Matsubara A, Futai K, Namba A, Shinkawa H (2006) Leupeptin, a calpain inhibitor, protects inner ear hair cells from aminoglycoside ototoxicity. Tohoku J Exp Med 209: 89-97. doi: 10.1620/tjem.209.89
Moral A, Navasa M, Rimola A, Garcia-Valdecasas JC, Grande L, Visa J, Rodes J (1994) Erythromycin ototoxicity in liver transplant patients. Transpl Int 7: 62-4. doi: 10.1007/BF00335665
Mount RJ, Takeno S, Wake M, Harrison RV (1995) Carboplatin ototoxicity in the chinchilla: lesions of the vestibular sensory epithelium. Acta Otolaryngol Suppl 519: 60-5. doi: 10.3109/00016489509121871
Musial-Bright L, Fengler R, Henze G, Hernaiz Driever P (2011) Carboplatin and ototoxicity: hearing loss rates among survivors of childhood medulloblastoma. Childs Nerv Syst 27: 407-13. doi: 10.1007/s00381-010-1300-1
Navarro-Ruiz NE (2020) Prevention of Platinum-Induced Hearing Loss in Children with Cancer. Am J Nurs 120: 21. doi: 10.1097/01.NAJ.0000668712.38501.b6
Nguyen T, Jeyakumar A (2019) Genetic susceptibility to aminoglycoside ototoxicity. Int J Pediatr Otorhinolaryngol 120: 15-19. doi: 10.1016/j.ijporl.2019.02.002
Nielsen-Abbring FW, Perenboom RM, van der Hulst RJ (1990) Quinine-induced hearing loss. ORL J Otorhinolaryngol Relat Spec 52: 65-8. doi: 10.1159/000276106
Nitz A, Kontopantelis E, Bielack S, Koscielniak E, Klingebiel T, Langer T, Paulides M (2013) Prospective evaluation of cisplatin- and carboplatin-mediated ototoxicity in paediatric and adult soft tissue and osteosarcoma patients. Oncol Lett 5: 311-315. doi: 10.3892/ol.2012.997
Niu P, Sun Y, Wang S, Li G, Tang X, Sun J, Pan C, Sun J (2021) Puerarin alleviates the ototoxicity of gentamicin by inhibiting the mitochondria‑dependent apoptosis pathway. Mol Med Rep 24. doi: 10.3892/mmr.2021.12491
Oh SY, Wasif N, Garcon MC, Rodriguez G, Saif MW (2013) Ototoxicity associated with oxaliplatin in a patient with pancreatic cancer. JOP 14: 676-9. doi: 10.6092/1590-8577/1629
Owusu E, Amartey BT, Afutu E, Boafo N (2022) Aminoglycoside Therapy for Tuberculosis: Evidence for Ototoxicity among Tuberculosis Patients in Ghana. Diseases 10. doi: 10.3390/diseases10010010
Paciello F, Fetoni AR, Mezzogori D, Rolesi R, Di Pino A, Paludetti G, Grassi C, Troiani D (2020) The dual role of curcumin and ferulic acid in counteracting chemoresistance and cisplatin-induced ototoxicity. Sci Rep 10: 1063. doi: 10.1038/s41598-020-57965-0
Paken J, Govender CD, Pillay M, Sewram V (2016) Cisplatin-Associated Ototoxicity: A Review for the Health Professional. J Toxicol 2016: 1809394. doi: 10.1155/2016/1809394
Paken J, Govender CD, Pillay M, Sewram V (2019) A Review of Cisplatin-Associated Ototoxicity. Semin Hear 40: 108-121. doi: 10.1055/s-0039-1684041
Parsons SK, Neault MW, Lehmann LE, Brennan LL, Eickhoff CE, Kretschmar CS, Diller LR (1998) Severe ototoxicity following carboplatin-containing conditioning regimen for autologous marrow transplantation for neuroblastoma. Bone Marrow Transplant 22: 669-74. doi: 10.1038/sj.bmt.1701391
Pavlidis P, Maurer J, Apostolidou E, Kekes G, Kouvelas D (2014) Memantine’s action against aminoglycoside-induced ototoxicity. Eur Arch Otorhinolaryngol 271: 1491-6. doi: 10.1007/s00405-013-2647-1
Peleg U, Perez R, Freeman S, Sohmer H (2007) Salicylate ototoxicity and its implications for cochlear microphonic potential generation. J Basic Clin Physiol Pharmacol 18: 173-88. doi: 10.1515/jbcpp.2007.18.3.173
Perletti G, Vral A, Patrosso MC, Marras E, Ceriani I, Willems P, Fasano M, Magri V (2008) Prevention and modulation of aminoglycoside ototoxicity (Review). Mol Med Rep 1: 3-13.
Pham TNM, Jeong SY, Kim DH, Park YH, Lee JS, Lee KW, Moon IS, Choung SY, Kim SH, Kang TH, Jeong KW (2020) Protective Mechanisms of Avocado Oil Extract Against Ototoxicity. Nutrients 12. doi: 10.3390/nu12040947
Qaddoumi I, Bass JK, Wu J, Billups CA, Wozniak AW, Merchant TE, Haik BG, Wilson MW, Rodriguez-Galindo C (2012) Carboplatin-associated ototoxicity in children with retinoblastoma. J Clin Oncol 30: 1034-41. doi: 10.1200/JCO.2011.36.9744
Qian ZJ, Alyono JC (2020) An association between marijuana use and tinnitus. Am J Otolaryngol 41: 102314. doi: 10.1016/j.amjoto.2019.102314
Ramu R, Sharma B, Karunakara D, Paliwal P, Bansal N, Taneja RS (2021) Liposomal amphotericin B-induced reversible ototoxicity in a patient with disseminated histoplasmosis. Indian J Pharmacol 53: 157-159. doi: 10.4103/0253-7613.316948
Rizzi MD, Hirose K (2007) Aminoglycoside ototoxicity. Curr Opin Otolaryngol Head Neck Surg 15: 352-7. doi: 10.1097/MOO.0b013e3282ef772d
Robler SK, Coco L, Krumm M (2022) Telehealth solutions for assessing auditory outcomes related to noise and ototoxic exposures in clinic and research. J Acoust Soc Am 152: 1737. doi: 10.1121/10.0013706
Ruhl D, Du TT, Wagner EL, Choi JH, Li S, Reed R, Kim K, Freeman M, Hashisaki G, Lukens JR, Shin JB (2019) Necroptosis and Apoptosis Contribute to Cisplatin and Aminoglycoside Ototoxicity. J Neurosci 39: 2951-2964. doi: 10.1523/JNEUROSCI.1384-18.2019
Rutka J (2019) Aminoglycoside Vestibulotoxicity. Adv Otorhinolaryngol 82: 101-110. doi: 10.1159/000490277
Rybak LP (1985) Furosemide ototoxicity: clinical and experimental aspects. Laryngoscope 95: 1-14. doi: 10.1288/00005537-198509010-00001
Rybak LP, Kelly T (2003) Ototoxicity: bioprotective mechanisms. Curr Opin Otolaryngol Head Neck Surg 11: 328-33. doi: 10.1097/00020840-200310000-00004
Rybak LP, Whitworth C (1986) Comparative ototoxicity of furosemide and piretanide. Acta Otolaryngol 101: 59-65. doi: 10.3109/00016488609108608
Rybak LP, Whitworth CA, Mukherjea D, Ramkumar V (2007) Mechanisms of cisplatin-induced ototoxicity and prevention. Hear Res 226: 157-67. doi: 10.1016/j.heares.2006.09.015
Sacristan JA, Angeles De Cos M, Soto J, Zurbano F, Pascual J, Tasis A, Valle R, De Pablos C (1993) Ototoxicity of erythromycin in man: electrophysiologic approach. Am J Otol 14: 186-8.
Sanchez VA, Shuey MM, Dinh PC, Jr., Monahan PO, Fossa SD, Sesso HD, Dolan ME, Einhorn LH, Vaughn DJ, Martin NE, Feldman DR, Kroenke K, Fung C, Frisina RD, Travis LB (2023) Patient-Reported Functional Impairment Due to Hearing Loss and Tinnitus After Cisplatin-Based Chemotherapy. J Clin Oncol 41: 2211-2226. doi: 10.1200/JCO.22.01456
Santos N, Ferreira RS, Santos ACD (2020) Overview of cisplatin-induced neurotoxicity and ototoxicity, and the protective agents. Food Chem Toxicol 136: 111079. doi: 10.1016/j.fct.2019.111079
Santucci NM, Garber B, Ivory R, Kuhn MA, Stephen M, Aizenberg D (2021) Insight into the current practice of ototoxicity monitoring during cisplatin therapy. J Otolaryngol Head Neck Surg 50: 19. doi: 10.1186/s40463-021-00506-0
Sass-Kortsak AM, Corey PN, Robertson JM (1995) An investigation of the association between exposure to styrene and hearing loss. Ann Epidemiol 5: 15-24. doi: 10.1016/1047-2797(94)00036-s
Schaper M, Demes P, Zupanic M, Blaszkewicz M, Seeber A (2003) Occupational toluene exposure and auditory function: results from a follow-up study. Ann Occup Hyg 47: 493-502. doi: 10.1093/annhyg/meg058
Schaper M, Seeber A, van Thriel C (2008) The effects of toluene plus noise on hearing thresholds: an evaluation based on repeated measurements in the German printing industry. Int J Occup Med Environ Health 21: 191-200. doi: 10.2478/v10001-008-0030-z
Schweitzer VG, Olson NR (1984) Ototoxic effect of erythromycin therapy. Arch Otolaryngol 110: 258-60. doi: 10.1001/archotol.1984.00800300050011
Sedo-Cabezon L, Boadas-Vaello P, Soler-Martin C, Llorens J (2014) Vestibular damage in chronic ototoxicity: a mini-review. Neurotoxicology 43: 21-27. doi: 10.1016/j.neuro.2013.11.009
Semedo MG, Dias-Silva N, Migueis J, Pita JR (2021) Quinine in Otology and Neurotology: Ototoxicity and Historic Role in Therapy. Otol Neurotol 42: 145-152. doi: 10.1097/MAO.0000000000002809
Shokoohi R, Khazaei M, Karami M, Seidmohammadi A, Berijani N, Khotanlou H, Torkshavand Z (2021) The relationship between chronic exposure to arsenic through drinking water and hearing function in exposed population aged 10-49 years: A cross-sectional study. Ecotoxicol Environ Saf 211: 111939. doi: 10.1016/j.ecoenv.2021.111939
Simpson TH, Schwan SA, Rintelmann WF (1992) Audiometric test criteria in the detection of cisplatin ototoxicity. J Am Acad Audiol 3: 176-85.
Simsek G, Tas BM, Muluk NB, Azman M, Kilic R (2019) Comparison of the protective efficacy between intratympanic dexamethasone and resveratrol treatments against cisplatin-induced ototoxicity: an experimental study. Eur Arch Otorhinolaryngol 276: 3287-3293. doi: 10.1007/s00405-019-05635-x
Singh Chauhan R, Saxena RK, Varshey S (2011) The role of ultrahigh-frequency audiometry in the early detection of systemic drug-induced hearing loss. Ear Nose Throat J 90: 218-22. doi: 10.1177/014556131109000506
Singh PK, Sharma V (2019) Ototoxicity, a rare but reversible adverse effect of a commonly used antimicrobial agent. BMJ Case Rep 12. doi: 10.1136/bcr-2019-230251
Skalleberg J, Myhrum M, Smastuen MC, Osnes TA, Fossa SD, Bunne M (2021) Speech perception 30 years after cisplatin-based chemotherapy in adults: limited clinical relevance of long-term ototoxicity? Acta Oncol 60: 426-433. doi: 10.1080/0284186X.2021.1887514
Skalleberg J, Smastuen MC, Oldenburg J, Osnes T, Fossa SD, Bunne M (2020) The Relationship Between Cisplatin-related and Age-related Hearing Loss During an Extended Follow-up. Laryngoscope 130: E515-E521. doi: 10.1002/lary.28543
Smyth D, Mossman S, Weatherall M, Jolliffe E, Joshi P, Taylor J, Thorne K, Watson E, Leadbetter R, Mossman B, Moss T, Todd N, Schneider E (2019) Gentamicin vestibulotoxicity with modern systemic dosing regimens: a prospective study using video-oculography. Acta Otolaryngol 139: 759-768. doi: 10.1080/00016489.2019.1637935
Sriyapai T, Thongyai K, Phuakpet K, Vathana N, Buaboonnam J, Sanpakit K (2022) Ototoxicity and long-term hearing outcome in pediatric patients receiving cisplatin. Turk J Pediatr 64: 531-541. doi: 10.24953/turkjped.2021.5012
Stevenson LJ, Biagio-de Jager L, Graham MA, Swanepoel W (2021) Community-Based Ototoxicity Monitoring for Drug-Resistant Tuberculosis in South Africa: An Evaluation Study. Int J Environ Res Public Health 18. doi: 10.3390/ijerph182111342
Steyger PS (2009) Potentiation of Chemical Ototoxicity by Noise. Semin Hear 30: 38-46. doi: 10.1055/s-0028-1111105
Steyger PS (2021) Mechanisms of Aminoglycoside- and Cisplatin-Induced Ototoxicity. Am J Audiol 30: 887-900. doi: 10.1044/2021_AJA-21-00006
Sturmer SH, Lechner A, Berking C (2021) Sudden Otovestibular Dysfunction in 3 Metastatic Melanoma Patients Treated With Immune Checkpoint Inhibitors. J Immunother 44: 193-197. doi: 10.1097/CJI.0000000000000367
Stypulkowski PH (1990) Mechanisms of salicylate ototoxicity. Hear Res 46: 113-45. doi: 10.1016/0378-5955(90)90144-e
Swanson DJ, Sung RJ, Fine MJ, Orloff JJ, Chu SY, Yu VL (1992) Erythromycin ototoxicity: prospective assessment with serum concentrations and audiograms in a study of patients with pneumonia. Am J Med 92: 61-8. doi: 10.1016/0002-9343(92)90016-5
Tan M, Toplu Y, Varan E, Sapmaz E, Ozhan O, Parlakpinar H, Polat A (2022) The effect of genistein on cisplatin induced ototoxicity and oxidative stress. Braz J Otorhinolaryngol 88: 105-111. doi: 10.1016/j.bjorl.2021.07.001
Tange RA, Dreschler WA, Claessen FA, Perenboom RM (1997) Ototoxic reactions of quinine in healthy persons and patients with Plasmodium falciparum infection. Auris Nasus Larynx 24: 131-6. doi: 10.1016/S0385-8146(96)00031-4
Tas BM, Simsek G, Azman M, Kilic R (2021) Efficacy of 2 Different Intratympanic Steroid Regimen on Prevention of Cisplatin Ototoxicity: An Experimental Study. Ear Nose Throat J 100: 417-422. doi: 10.1177/0145561319874311
Terzi S, Ozgur A, Celiker M, Mercantepe T, Yilmaz A, Tumkaya L, Kaya S, Demir E, Dursun E (2021) The protective effect of astaxanthin on cisplatin-induced ototoxicity. Adv Clin Exp Med 30: 315-321. doi: 10.17219/acem/133081
Thompson P, Wood RP, 2nd, Bergstrom L (1980) Erythromycin ototoxicity. J Otolaryngol 9: 60-2.
Traber PG, Levine DP (1981) Vancomycin Ototoxicity in patient with normal renal function. Ann Intern Med 95: 458-60. doi: 10.7326/0003-4819-95-4-458
Tserga E, Moreno-Paublete R, Sarlus H, Bjorn E, Guimaraes E, Goritz C, Cederroth CR, Canlon B (2020) Circadian vulnerability of cisplatin-induced ototoxicity in the cochlea. FASEB J 34: 13978-13992. doi: 10.1096/fj.202001236R
Tserga E, Nandwani T, Edvall NK, Bulla J, Patel P, Canlon B, Cederroth CR, Baguley DM (2019) The genetic vulnerability to cisplatin ototoxicity: a systematic review. Sci Rep 9: 3455. doi: 10.1038/s41598-019-40138-z
Tsuji K, Velazquez-Villasenor L, Rauch SD, Glynn RJ, Wall C, 3rd, Merchant SN (2000) Temporal bone studies of the human peripheral vestibular system. Aminoglycoside ototoxicity. Ann Otol Rhinol Laryngol Suppl 181: 20-5. doi: 10.1177/00034894001090s504
Turan C, Kantar M, Aktan C, Kosova B, Orman M, Bilgen C, Kirazli T (2019) Cisplatin ototoxicity in children: risk factors and its relationship with polymorphisms of DNA repair genes ERCC1, ERCC2, and XRCC1. Cancer Chemother Pharmacol 84: 1333-1338. doi: 10.1007/s00280-019-03968-2
Tuzel IH (1981) Comparison of adverse reactions to bumetanide and furosemide. J Clin Pharmacol 21: 615-9. doi: 10.1002/j.1552-4604.1981.tb05673.x
van der Hulst RJ, Boeschoten EW, Nielsen FW, Struijk DG, Dreschler WD, Tange RA (1991) Ototoxicity monitoring with ultra-high frequency audiometry in peritoneal dialysis patients treated with vancomycin or gentamicin. ORL J Otorhinolaryngol Relat Spec 53: 19-22. doi: 10.1159/000276178
van Marion WF, van der Meer JW, Kalff MW, Schicht SM (1978) Ototoxicity of erythromycin. Lancet 2: 214-5. doi: 10.1016/s0140-6736(78)91961-x
Veiga M, Kuhweide R, Demaerel V, De Pauw R, De Foer B, Casselman JW (2021) Labyrinthine enhancement on 3D black blood MR images of the brain as an imaging biomarker for cisplatin ototoxicity in (lung) cancer patients. Neuroradiology 63: 81-90. doi: 10.1007/s00234-020-02504-x
Vietor NO, George BJ (2012) Oxaliplatin-induced hepatocellular injury and ototoxicity: a review of the literature and report of unusual side effects of a commonly used chemotherapeutic agent. J Oncol Pharm Pract 18: 355-9. doi: 10.1177/1078155212437901
Voogt GR, Schoeman HS (1996) Ototoxicity of aminoglycoside drugs in tuberculosis treatment. S Afr J Commun Disord 43: 3-6.
Waissbluth S (2020) Is Cyclosporine Ototoxic? Front Neurol 11: 593917. doi: 10.3389/fneur.2020.593917
Waissbluth S, Chuang A, Del Valle A, Cordova M (2018) Long term platinum-induced ototoxicity in pediatric patients. Int J Pediatr Otorhinolaryngol 107: 75-79. doi: 10.1016/j.ijporl.2018.01.028
Waissbluth S, Peleva E, Daniel SJ (2017) Platinum-induced ototoxicity: a review of prevailing ototoxicity criteria. Eur Arch Otorhinolaryngol 274: 1187-1196. doi: 10.1007/s00405-016-4117-z
Wallace MR, Miller LK, Nguyen MT, Shields AR (1994) Ototoxicity with azithromycin. Lancet 343: 241. doi: 10.1016/s0140-6736(94)91030-8
Wanamaker HH, Slepecky NB, Cefaratti LK, Ogata Y (1999) Comparison of vestibular and cochlear ototoxicity from transtympanic streptomycin administration. Am J Otol 20: 457-64.
Wang N, Xu A, Zhang H, Zhang Y, Sui R, Fan X, Hou L, Shi L (2022) Melatonin Attenuates Cisplatin-Induced Ototoxicity via Regulating the Cell Apoptosis of the Inner Ear. Comput Math Methods Med 2022: 7160816. doi: 10.1155/2022/7160816
Warchol ME (2010) Cellular mechanisms of aminoglycoside ototoxicity. Curr Opin Otolaryngol Head Neck Surg 18: 454-8. doi: 10.1097/MOO.0b013e32833e05ec
Ward KM, Rounthwaite FJ (1978) Neomycin ototoxicity. Ann Otol Rhinol Laryngol 87: 211-5. doi: 10.1177/000348947808700211
Watts KL (2019) Ototoxicity: Visualized in Concept Maps. Semin Hear 40: 177-187. doi: 10.1055/s-0039-1684046
Wen Y, Zong S, Liu T, Du P, Li H, Xiao H (2021) Tauroursodeoxycholic acid attenuates cisplatin-induced ototoxicity by inhibiting the accumulation and aggregation of unfolded or misfolded proteins in the endoplasmic reticulum. Toxicology 453: 152736. doi: 10.1016/j.tox.2021.152736
Wen YH, Lin HY, Lin JN, Tseng GF, Hwang CF, Lin CC, Hsu CJ, Wu HP (2022) 2,3,4′,5‑Tetrahydroxystilbene‑2‑O‑beta‑D‑glucoside ameliorates gentamicin‑induced ototoxicity by modulating autophagy via Sesn2/AMPK/mTOR signaling. Int J Mol Med 49. doi: 10.3892/ijmm.2022.5127
Wu P, Wu X, Zhang C, Chen X, Huang Y, Li H (2021) Hair Cell Protection from Ototoxic Drugs. Neural Plast 2021: 4909237. doi: 10.1155/2021/4909237
Xuan L, Sun B, Meng X, Liu C, Cong Y, Wu S (2020) Ototoxicity in patients with invasive ductal breast cancer who were treated with docetaxel: report of two cases. Cancer Biol Ther 21: 990-993. doi: 10.1080/15384047.2020.1831370
Yildirim A, Fidan E, Ozdemir F (2022) Hearing Loss After the First Low Dose Administration of Cisplatin. J Coll Physicians Surg Pak 32: 1216-1218. doi: 10.29271/jcpsp.2022.09.1216
Yurtsever KN, Baklaci D, Guler I, Kuzucu I, Kum RO, Ozhamam EU, Ozcan M, Dere H (2020) The Protective Effect of Platelet Rich Plasma Against Cisplatin-Induced Ototoxicity. J Craniofac Surg 31: e506-e509. doi: 10.1097/SCS.0000000000006645
Zadrozniak M, Szymanski M, Luszczki JJ (2019) Vitamin C alleviates ototoxic effect caused by coadministration of amikacin and furosemide. Pharmacol Rep 71: 351-356. doi: 10.1016/j.pharep.2019.01.002
Zhang W, Xiong H, Pang J, Su Z, Lai L, Lin H, Jian B, He W, Yang H, Zheng Y (2020) Nrf2 activation protects auditory hair cells from cisplatin-induced ototoxicity independent on mitochondrial ROS production. Toxicol Lett 331: 1-10. doi: 10.1016/j.toxlet.2020.04.005
Zhang X, Yu J (2019) Baicalin attenuates gentamicin-induced cochlear hair cell ototoxicity. J Appl Toxicol 39: 1208-1214. doi: 10.1002/jat.3806
Zhang Y, Lv Z, He Q (2022) Agmatine Alleviates Cisplatin-Induced Ototoxicity by Activating PI3K/AKT Signaling Pathway. eNeuro 9. doi: 10.1523/ENEURO.0434-21.2022
Zheng Z, Tang D, Zhao L, Li W, Han J, Hu B, Nie G, He Y (2020a) Liproxstatin-1 Protects Hair Cell-Like HEI-OC1 Cells and Cochlear Hair Cells against Neomycin Ototoxicity. Oxid Med Cell Longev 2020: 1782659. doi: 10.1155/2020/1782659
Zheng Z, Wang Y, Yu H, Li W, Wu J, Cai C, He Y (2020b) Salvianolic acid B inhibits ototoxic drug-induced ototoxicity by suppression of the mitochondrial apoptosis pathway. J Cell Mol Med 24: 6883-6897. doi: 10.1111/jcmm.15345
Zong Y, Chen F, Li S, Zhang H (2021) (-)-Epigallocatechin-3-gallate (EGCG) prevents aminoglycosides-induced ototoxicity via anti-oxidative and anti-apoptotic pathways. Int J Pediatr Otorhinolaryngol 150: 110920. doi: 10.1016/j.ijporl.2021.110920
![]()