By Marcello Cherchi, MD PhD
Introduction
The diagnostic tests that have made their way into clinical use generally meet several criteria:
- They are helpful in diagnosing multiple diseases, including some which are common.
- They are affordable by a clinical practice.
- They physically fit into a clinical practice.
Below we briefly discuss some tools that are relevant for testing vestibular system function, but fail to meet one or more of the criteria listed above.
Human centrifuge
Human centrifuges are a mechanism for using the centrifugal component of rotational acceleration to mimic linear acceleration (Brandt 1962; Hallgren et al. 2016; Hallgren et al. 2015; Moore et al. 2003; Schoenmaekers et al. 2022). The linear acceleration can be used to study otolith function.
The Figure below, from Hallgren and colleagues (Hallgren et al. 2015), illustrates an experimental human centrifuge setup.
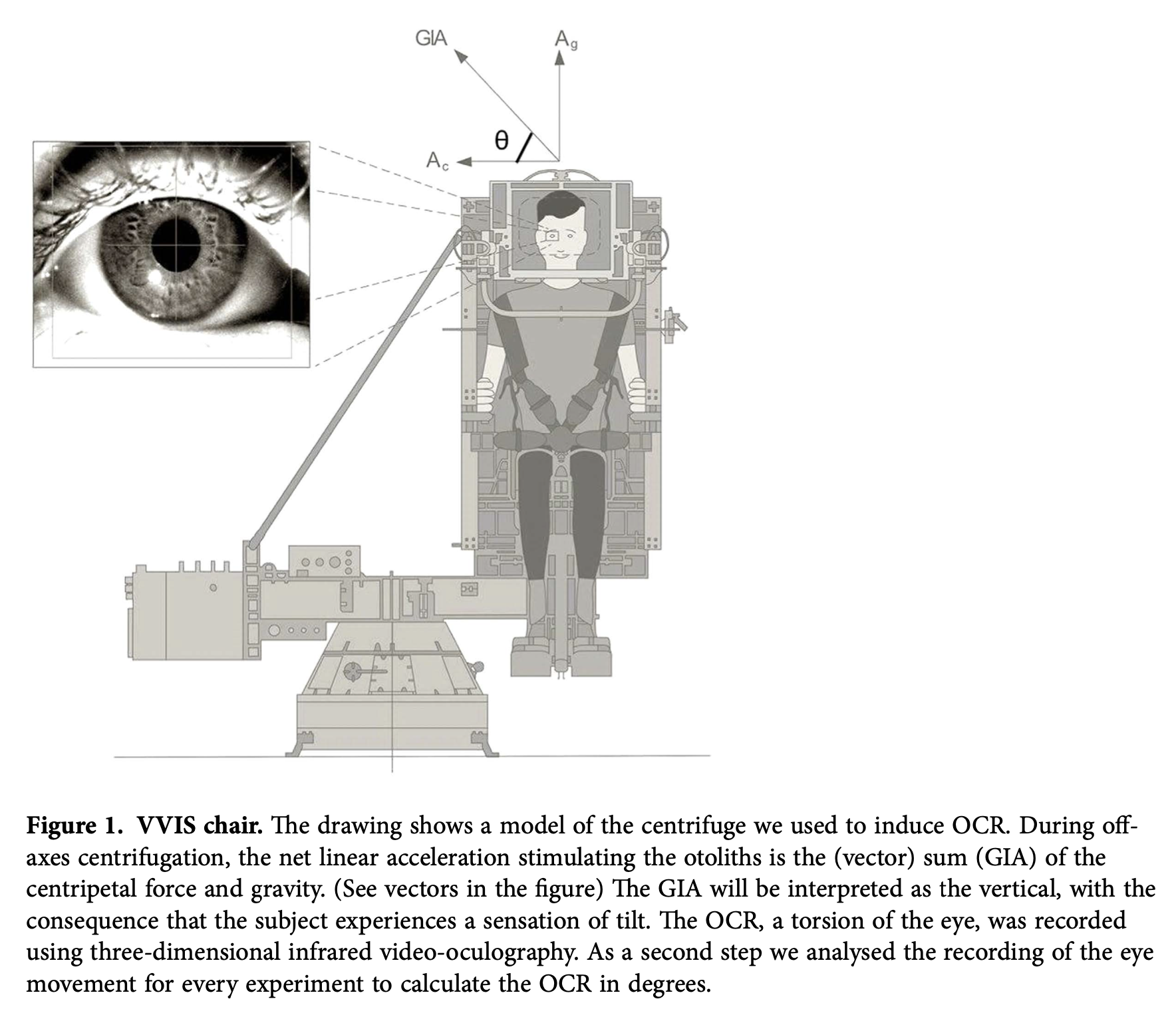
The Figure below, from Schoenmaekers and colleagues (Schoenmaekers et al. 2022), illustrates a setup used for utricular stimulation.
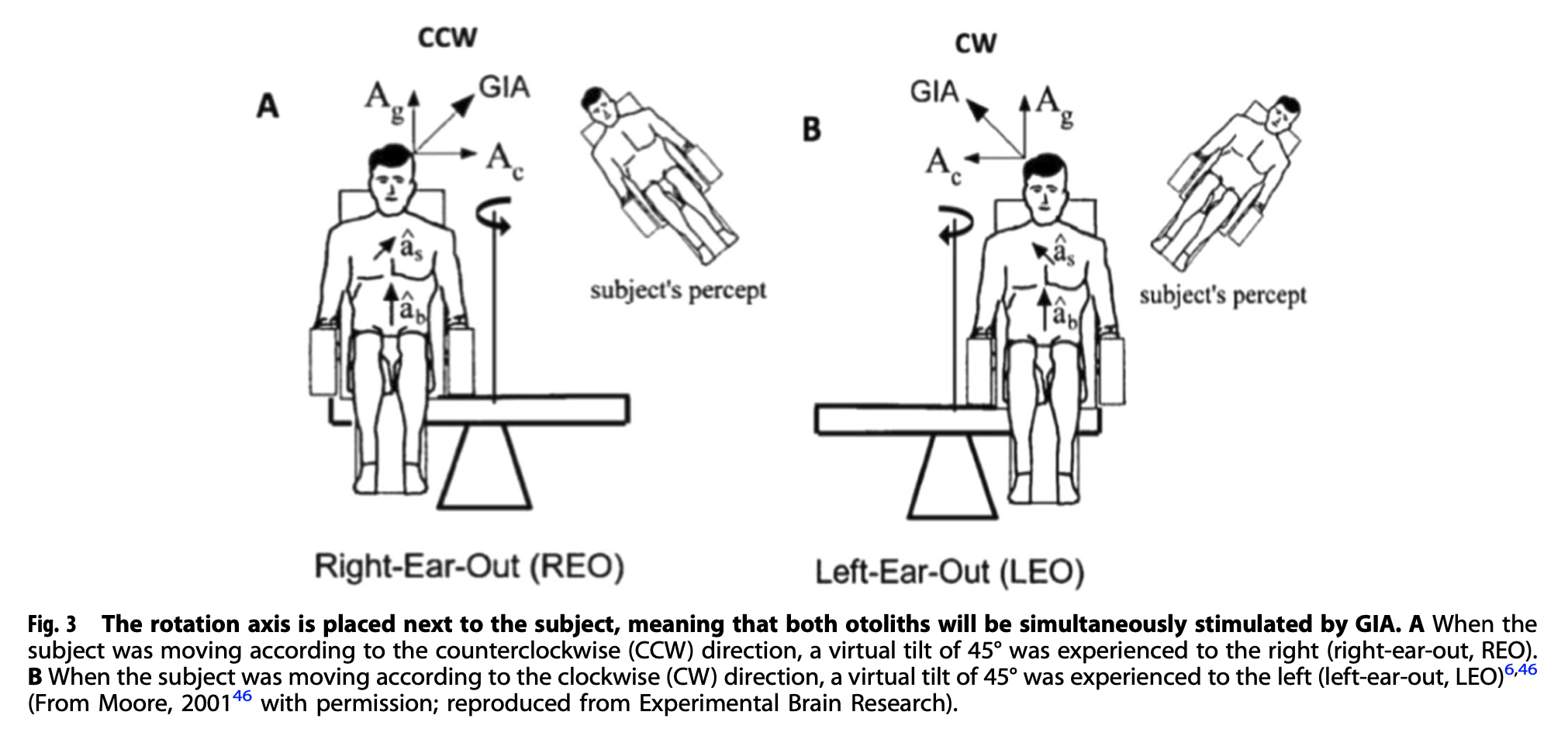
The arrangements shown in the figures above can be achieved with a modified rotatory chair. More elaborate human centrifuges with swinging gondolas have also been used, as shown in the Figure below, from Tribukait and Eiken (Tribukait and Eiken 2005).
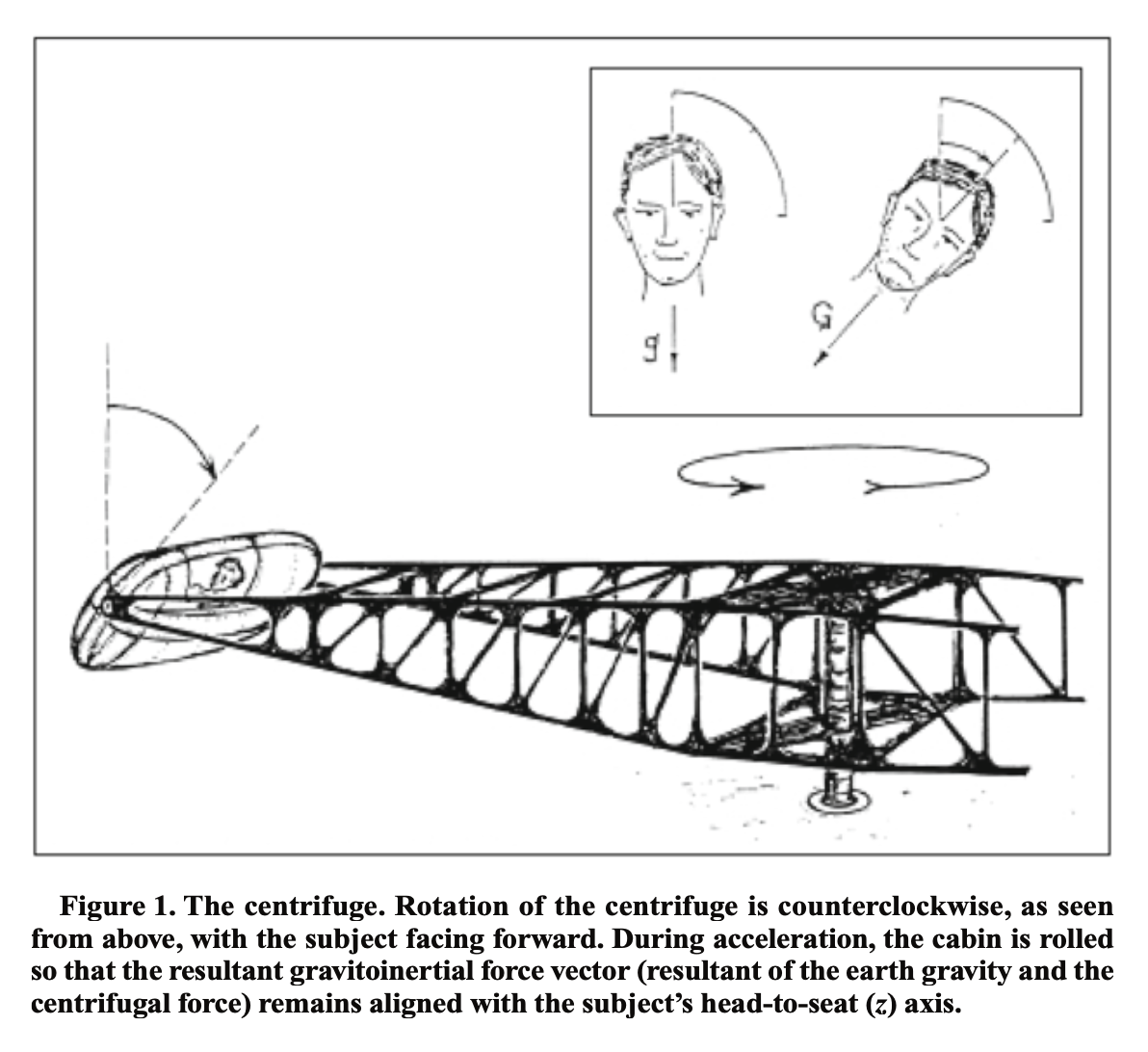
Customized rotatory chair setups are expensive. Human centrifuges with swinging gondolas are expensive and take up a great deal of space.
Moog platform
William Moog (1915 – 1997) invented the electrohydraulic servo valve, which was one of the crucial components in developing the Moog platform. This device is helpful in studying vestibular responses to static and dynamic tilt.
The Figures below, from Mardirossian and colleagues (Mardirossian et al. 2014), and from Strupp and colleagues (Strupp et al. 2023), show Moog platforms.
 |
 |
Moog platforms are expensive pieces of machinery that require considerable space, and consequently are largely restricted to research settings, so there is relatively little literature drawing on data from them (Beylergil et al. 2019; Chaudhuri et al. 2013; La Scaleia et al. 2023; Mardirossian et al. 2014).
Parallel swing
Parallel swing testing is a method for testing otolith responses to linear acceleration.
The Figures below, from Gresty and Bronstein (Gresty and Bronstein 1992) and Walsh (Walsh 1961), show a schematics of the arrangement of a parallel swing.
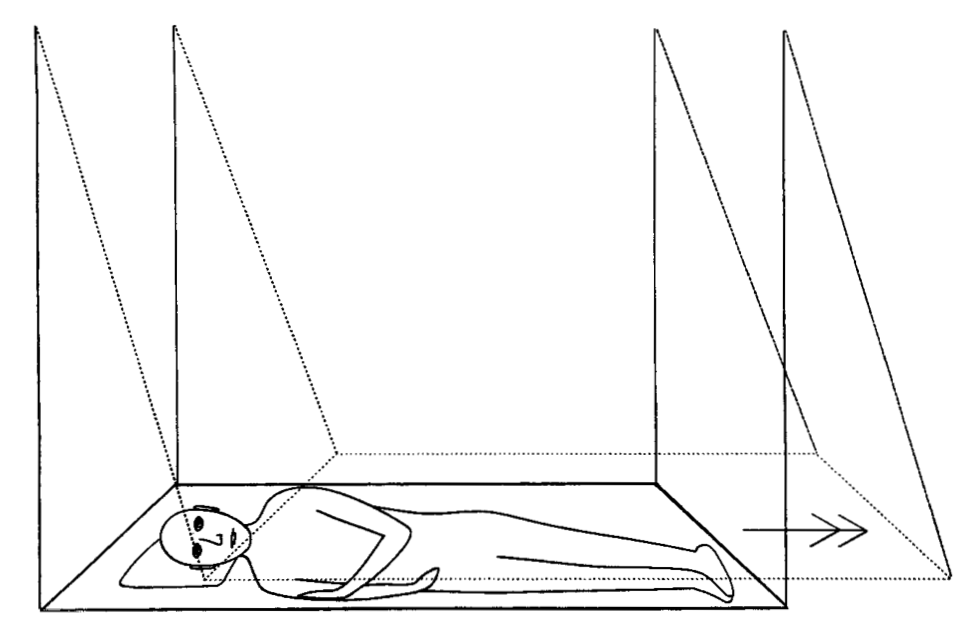 |
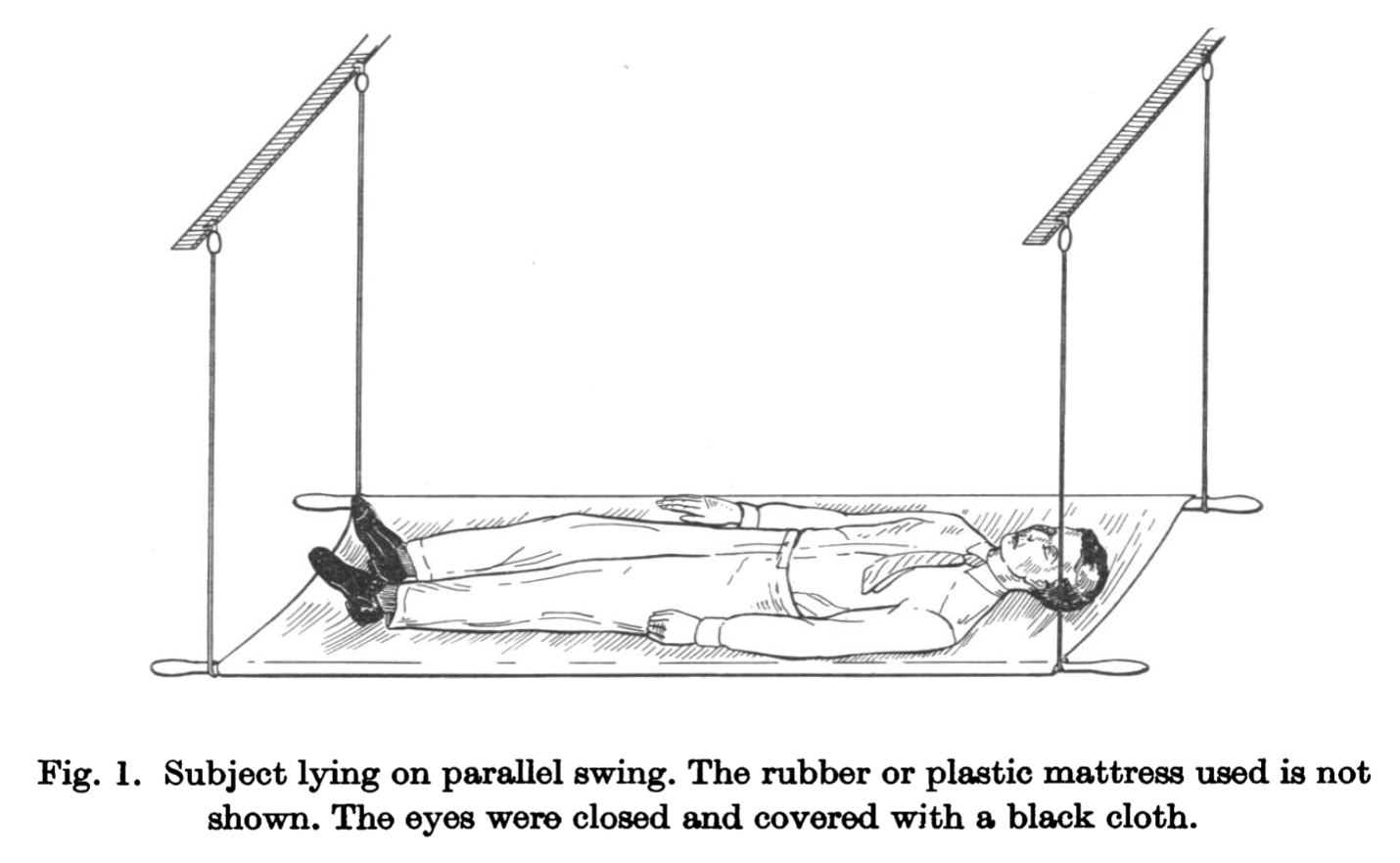 |
In practice, parallel swings are quite large, as shown in the Figures below, from Oosterveld (Oosterveld 1970) and Greven and colleagues (Greven et al. 1974).
 |
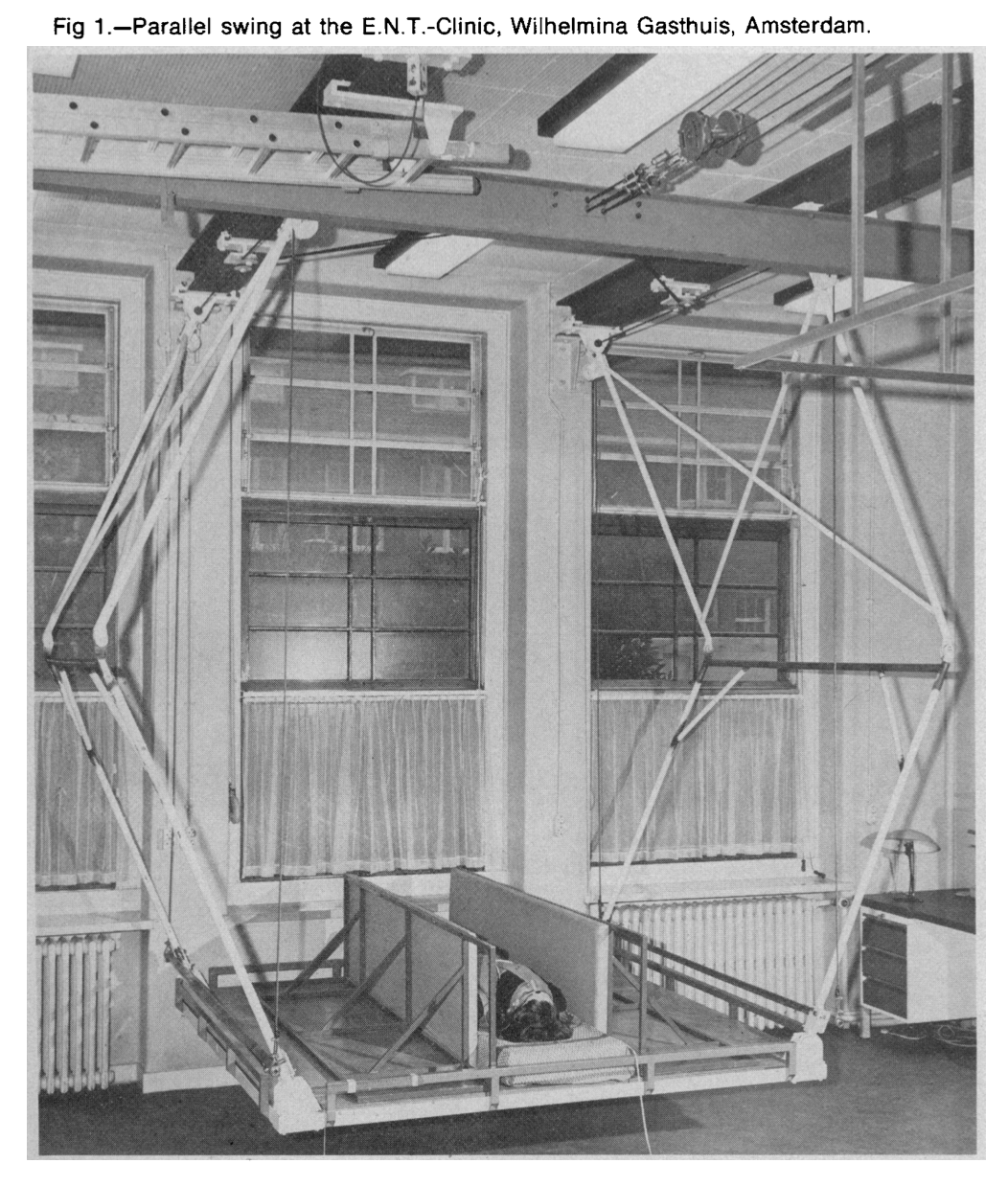 |
Parallel swings require considerable space for operation.
Linear accelerator (“sled”)
Sleds (also called linear accelerators) have been used to generate linear acceleration for testing otolith function.
The Figure below, from Gresty and Bronstein (Gresty and Bronstein 1992), shows the setup of a sled for this purpose.

These types of devices are generally constructed in research laboratories.
Gait analysis
Gait analysis involves tracking in two or three dimensions the movement of individual joints during locomotion. This is generally done in a gait lab, which requires a complex setup for capturing and analyzing data.
The Figures below, from Pamies-Vila and colleagues (Pàmies-Vilà et al. 2015), show examples of fiducial marking of joints, and the cameras that track their movements.
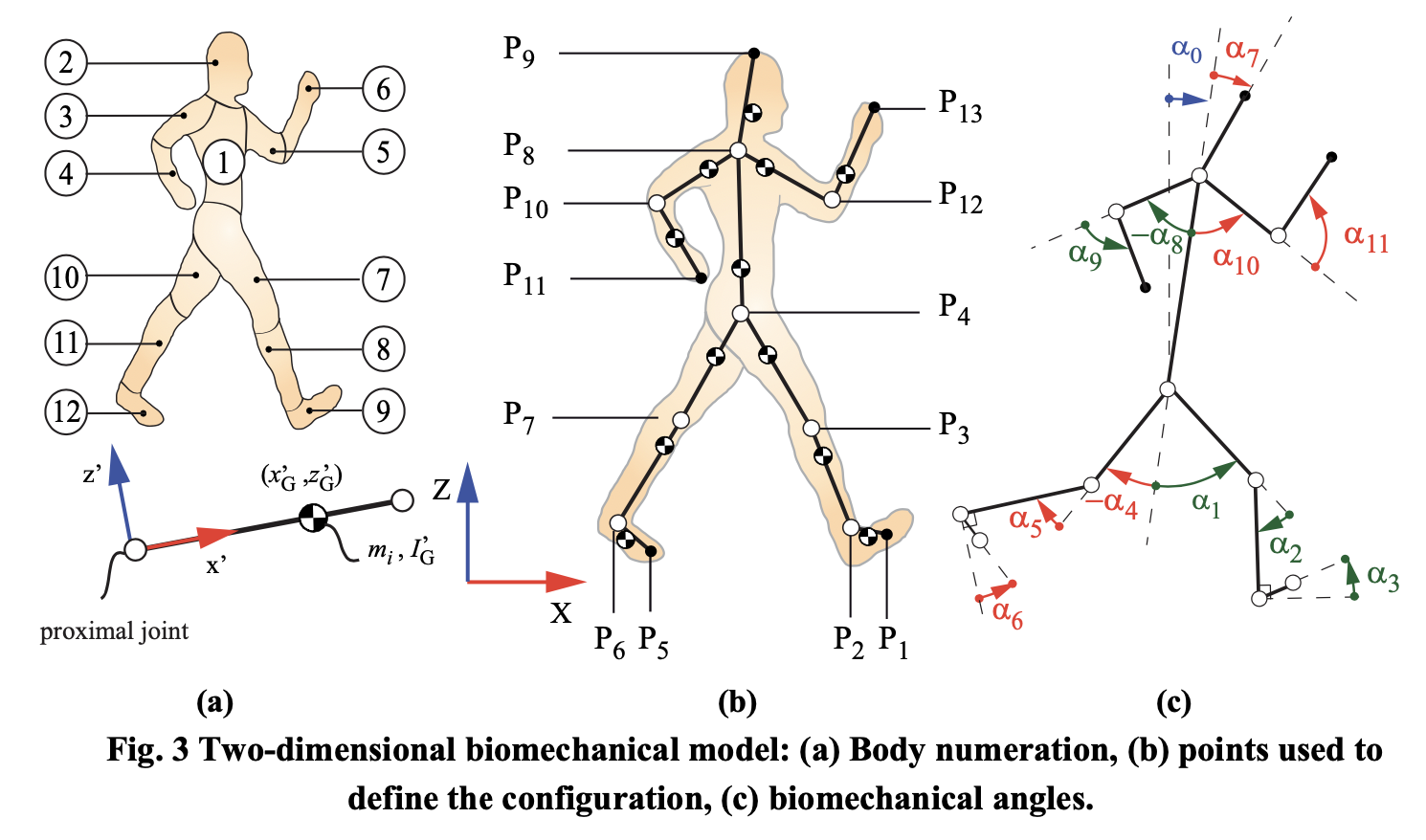 |
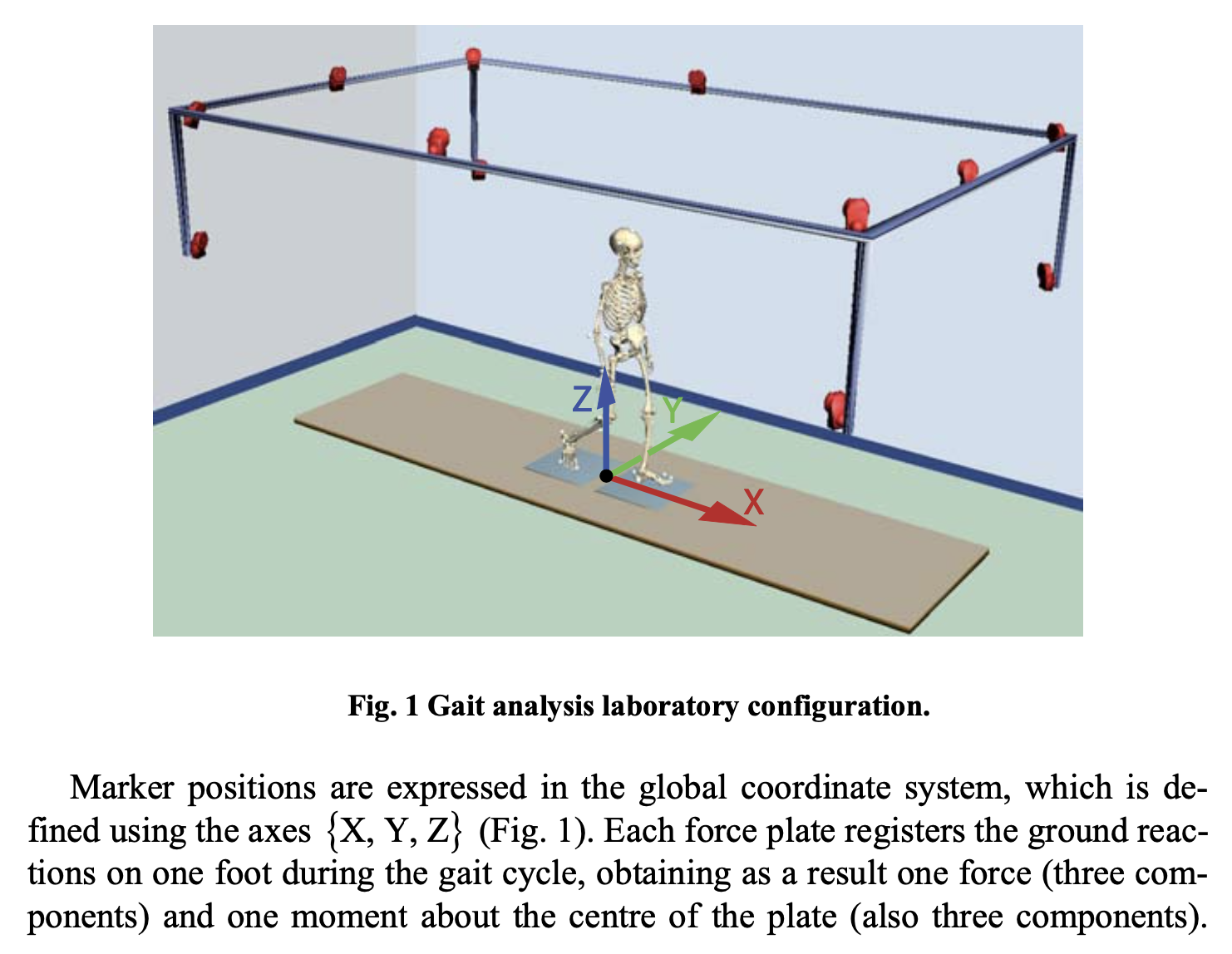 |
Gait laboratories are expensive operations that require considerable computing power for data collection and analysis.
Wearable inertial sensors
The miniaturization of technology for sensors (accelerometers) and transmitters (WiFi, Bluetooth) has advanced application of wearable inertial sensors for clinical research. Much of this remains restricted to investigational protocols, but it is likely that this will gradually penetrate medical practice in fields such as ataxia (Shah et al. 2021; Velazquez-Perez et al. 2021; Zhou et al. 2022) and movement disorders (Carpinella et al. 2017; Hubble et al. 2015; Lu et al. 2020; Monje et al. 2019; Ossig et al. 2016; Pardoel et al. 2019; Sanchez-Ferro and Maetzler 2016). This technology is just beginning to be applied to vestibular disorders (AlSharif et al. 2023; Gawronska et al. 2023; Gawronska et al. 2022; Meldrum et al. 2022; Zhang et al. 2021).
References
AlSharif DS, Tucker CA, Coffman DL, Keshner EA (2023) Electrodermal and postural responses in dizzy adults: Diagnostic indicators of vestibular migraine. J Vestib Res 33: 51-62. doi: 10.3233/VES-220004
Beylergil SB, Karmali F, Wang W, Bermudez Rey MC, Merfeld DM (2019) Vestibular roll tilt thresholds partially mediate age-related effects on balance. Prog Brain Res 248: 249-267. doi: 10.1016/bs.pbr.2019.04.019
Brandt U (1962) Reorientation and vestibular function. A comparison in the human centrifuge between fighter pilots and non-aviators. Acta Otolaryngol 54: 543-52.
Carpinella I, Cattaneo D, Bonora G, Bowman T, Martina L, Montesano A, Ferrarin M (2017) Wearable Sensor-Based Biofeedback Training for Balance and Gait in Parkinson Disease: A Pilot Randomized Controlled Trial. Arch Phys Med Rehabil 98: 622-630 e3. doi: 10.1016/j.apmr.2016.11.003
Chaudhuri SE, Karmali F, Merfeld DM (2013) Whole body motion-detection tasks can yield much lower thresholds than direction-recognition tasks: implications for the role of vibration. J Neurophysiol 110: 2764-72. doi: 10.1152/jn.00091.2013
Gawronska A, Rosiak O, Pajor A, Janc M, Kotas R, Kaminski M, Zamyslowska-Szmytke E, Jozefowicz-Korczynska M (2023) Instrumental and Non-Instrumental Measurements in Patients with Peripheral Vestibular Dysfunctions. Sensors (Basel) 23. doi: 10.3390/s23041994
Gawronska A, Zamyslowska-Szmytke E, Janc M, Kotas R, Kaminski M, Marciniak P, Tylman W, Wozniak S, Napieralski J, Sakowicz B, Pajor A, Rosiak O, Puzio A, Lucas-Brot W, Jozefowicz-Korczynska M (2022) Innovative System for Evaluation and Rehabilitation of Human Imbalance. Otolaryngol Pol 76: 7-11. doi: 10.5604/01.3001.0015.7927
Gresty MA, Bronstein AM (1992) Testing otolith function. Br J Audiol 26: 125-36. doi: 10.3109/03005369209077880
Greven AJ, Oosterveld WJ, Rademakers WJ (1974) Linear acceleration perception: threshold determinations with the use of a parallel swing. Arch Otolaryngol 100: 453-9. doi: 10.1001/archotol.1974.00780040467009
Hallgren E, Kornilova L, Fransen E, Glukhikh D, Moore ST, Clement G, Van Ombergen A, MacDougall H, Naumov I, Wuyts FL (2016) Decreased otolith-mediated vestibular response in 25 astronauts induced by long-duration spaceflight. J Neurophysiol 115: 3045-51. doi: 10.1152/jn.00065.2016
Hallgren E, Migeotte PF, Kornilova L, Deliere Q, Fransen E, Glukhikh D, Moore ST, Clement G, Diedrich A, MacDougall H, Wuyts FL (2015) Dysfunctional vestibular system causes a blood pressure drop in astronauts returning from space. Sci Rep 5: 17627. doi: 10.1038/srep17627
Hubble RP, Naughton GA, Silburn PA, Cole MH (2015) Wearable sensor use for assessing standing balance and walking stability in people with Parkinson’s disease: a systematic review. PLoS One 10: e0123705. doi: 10.1371/journal.pone.0123705
La Scaleia B, Lacquaniti F, Zago M (2023) Enhancement of Vestibular Motion Discrimination by Small Stochastic Whole-body Perturbations in Young Healthy Humans. Neuroscience 510: 32-48. doi: 10.1016/j.neuroscience.2022.12.010
Lu R, Xu Y, Li X, Fan Y, Zeng W, Tan Y, Ren K, Chen W, Cao X (2020) Evaluation of Wearable Sensor Devices in Parkinson’s Disease: A Review of Current Status and Future Prospects. Parkinsons Dis 2020: 4693019. doi: 10.1155/2020/4693019
Mardirossian V, Karmali F, Merfeld D (2014) Thresholds for human perception of roll tilt motion: patterns of variability based on visual, vestibular, and mixed cues. Otol Neurotol 35: 857-60. doi: 10.1097/MAO.0000000000000346
Meldrum D, Murray D, Vance R, Coleman S, McConnell S, Hardiman O, McConn Walsh R (2022) Toward a Digital Health Intervention for Vestibular Rehabilitation: Usability and Subjective Outcomes of a Novel Platform. Front Neurol 13: 836796. doi: 10.3389/fneur.2022.836796
Monje MHG, Foffani G, Obeso J, Sanchez-Ferro A (2019) New Sensor and Wearable Technologies to Aid in the Diagnosis and Treatment Monitoring of Parkinson’s Disease. Annu Rev Biomed Eng 21: 111-143. doi: 10.1146/annurev-bioeng-062117-121036
Moore ST, Clement G, Dai M, Raphan T, Solomon D, Cohen B (2003) Ocular and perceptual responses to linear acceleration in microgravity: alterations in otolith function on the COSMOS and Neurolab flights. J Vestib Res 13: 377-93.
Oosterveld WJ (1970) The parallel swing. Arch Otolaryngol 91: 154-7. doi: 10.1001/archotol.1970.00770040224009
Ossig C, Antonini A, Buhmann C, Classen J, Csoti I, Falkenburger B, Schwarz M, Winkler J, Storch A (2016) Wearable sensor-based objective assessment of motor symptoms in Parkinson’s disease. J Neural Transm (Vienna) 123: 57-64. doi: 10.1007/s00702-015-1439-8
Pàmies-Vilà R, Font-Llagunes J, Lugrís U, Alonso F, Cuadrado J (2015) A Computational Benchmark for 2D Gait Analysis Problems. Mechanisms and Machine Science 24: 689-697. doi: 10.1007/978-3-319-09411-3_73
Pardoel S, Kofman J, Nantel J, Lemaire ED (2019) Wearable-Sensor-based Detection and Prediction of Freezing of Gait in Parkinson’s Disease: A Review. Sensors (Basel) 19. doi: 10.3390/s19235141
Sanchez-Ferro A, Maetzler W (2016) Advances in sensor and wearable technologies for Parkinson’s disease. Mov Disord 31: 1257. doi: 10.1002/mds.26746
Schoenmaekers C, De Laet C, Kornilova L, Glukhikh D, Moore S, MacDougall H, Naumov I, Fransen E, Wille L, Jillings S, Wuyts FL (2022) Ocular counter-roll is less affected in experienced versus novice space crew after long-duration spaceflight. NPJ Microgravity 8: 27. doi: 10.1038/s41526-022-00208-5
Shah VV, Rodriguez-Labrada R, Horak FB, McNames J, Casey H, Hansson Floyd K, El-Gohary M, Schmahmann JD, Rosenthal LS, Perlman S, Velazquez-Perez L, Gomez CM (2021) Gait Variability in Spinocerebellar Ataxia Assessed Using Wearable Inertial Sensors. Mov Disord 36: 2922-2931. doi: 10.1002/mds.28740
Strupp M, Brandt T, Dieterich M (2023) Mal de Débarquement Syndrome. In: Strupp M, Brandt T, Dieterich M (eds) Vertigo and Dizziness: Common Complaints. Springer International Publishing, Cham, pp 359-363
Tribukait A, Eiken O (2005) On the role of otoliths and semicircular canals in spatial orientation: Dynamics of the visually perceived eye level during gondola centrifugation. Percept Psychophys 67: 1242-51. doi: 10.3758/bf03193556
Velazquez-Perez L, Rodriguez-Labrada R, Gonzalez-Garces Y, Arrufat-Pie E, Torres-Vega R, Medrano-Montero J, Ramirez-Bautista B, Vazquez-Mojena Y, Auburger G, Horak F, Ziemann U, Gomez CM (2021) Prodromal Spinocerebellar Ataxia Type 2 Subjects Have Quantifiable Gait and Postural Sway Deficits. Mov Disord 36: 471-480. doi: 10.1002/mds.28343
Walsh EG (1961) Role of the vestibular apparatus in the perception of motion on a parallel swing. J Physiol 155: 506-13. doi: 10.1113/jphysiol.1961.sp006643
Zhang Y, Wang H, Yao Y, Liu J, Sun X, Gu D (2021) Walking stability in patients with benign paroxysmal positional vertigo: an objective assessment using wearable accelerometers and machine learning. J Neuroeng Rehabil 18: 56. doi: 10.1186/s12984-021-00854-y
Zhou H, Nguyen H, Enriquez A, Morsy L, Curtis M, Piser T, Kenney C, Stephen CD, Gupta AS, Schmahmann JD, Vaziri A (2022) Assessment of gait and balance impairment in people with spinocerebellar ataxia using wearable sensors. Neurol Sci 43: 2589-2599. doi: 10.1007/s10072-021-05657-6
![]()