By Marcello Cherchi, MD PhD
For patients
A glomus tympanicum (GT) is a vascular tumor in the middle ear, usually in just one ear. It is more common in adults, and more common in women. Over half of cases cause pulsatile tinnitus, and about a third of cases cause hearing loss. If you have these symptoms, and if your physician sees a red pulsatile mass behind your eardrum, then you will be referred to an otolaryngologist (ENT), who may order imaging studies to confirm the diagnosis. Depending on the location and extent of the GT, the ENT may consider surgery, or radiation therapy, or a combination. GTs do not usually recur.
For clinicians
Overview
A glomus tympanicum (GT) tumor is a paraganglioma arising at various locations in the middle ear. It is highly vascular, and the classic appearance under otomicroscopy/otoscopy is a red pulsatile mass behind the eardrum. It is usually a disease of adulthood, and is more common in women. A number of diseases can resemble GTs, and GTs can mimic other lesions. About 15% of GTs secrete catecholamines. The most common presenting symptoms are pulsatile tinnitus and hearing loss. Rarely GTs can cause disequilibrium and epistaxis. GTs are usually unilateral; they can occur with other paragangliomas anywhere along the sympathetic chain. Audiometry usually shows mixed conductive and sensorineural hearing loss. CT is usually the imaging modality of choice, but MRI and various forms of angiography may also play a role. Treatment is usually surgical, though radiation therapy has become more common. Recurrence is uncommon, and occurs more frequently in surgically-treated cases. If a clinician observes a red pulsatile mass behind the eardrum, referral to a neuro-otologic otolaryngologist is appropriate.
Introduction
Glomus tympanicum (GT) tumors are a type of paraganglioma.
“Extra-adrenal paragangliomas (PGOMAs) are rare and can occur anywhere along the sympathetic chain including the carotid body, glomus jugulare, vagal bodies, ganglium tympanicum, larynx, ciliary bodies, organs of Zuckerkandl, urinary bladder, and other locations” (Snitzer, Sheeler et al. 1995).
Embryologically, paragangliomas originate from non-chromaffin (Neto, Vuono et al. 2005) neural crest cells (Mafee, Raofi et al. 2000, Fountarlis, Hajiioannou et al. 2022) of the autonomic nervous system (Ma, Ji et al. 2012).
Of particular interest in neuro-otology are paragangliomas arising from the tympanic membrane; these are usually called “glomus tympanicum” (GT) tumors, and “are benign arising from paraganglion cells of the tympanic plexus in the middle ear” (Sweeney, Carlson et al. 2015) “located on promontory” (Fountarlis, Hajiioannou et al. 2022).
Terminology
The term “glomus” derives from a Latin word usually translated as “ball of yarn,” reflecting the vascular nature of these lesions.
Sometimes paragangliomas are referred to as “glomus tumors,” but some authors reserve the term “glomus tumor” to refer to “hyperplasia of glomus bodies” rather than to paragangliomas (Wieser, Gilley et al. 2022).
Histopathology
Despite the common embryologic origin, GTs differ histopathologically from other paragangliomas (Branica, Sprem et al. 1993).
Pathophysiology
GTs cause symptoms by virtue of occupying the middle ear space (where they can impinge on the ossicular chain and cause conductive hearing loss) and invasion into other areas, and by virtue of the fact that they are heavily vascularized (and thus can produce pulsatile tinnitus).
A minority of GTs secrete catecholamines. Anand and colleagues report 15% of GTs to be secreting (Anand, Leonetti et al. 1993). In such cases, laboratory studies may detect elevated levels of noradrenalin in the serum, and vanillylmandelic acid in the urine (Kouzaki, Fukui et al. 2008).
Laterality
GTs usually present unilaterally, but cases of bilateral involvement have been reported (Fukushima, Hara et al. 2018).
Co-occurrence with other paragangliomas
GT can occur with other paragangliomas, such as glomus vagale and glomus jugulare (Balatsouras, Eliopoulos et al. 1992), or with glomus of the carotid body (Balatsouras, Eliopoulos et al. 1992).
Epidemiology
GT is primarily a disease of adults, but has also been reported in children (Busby and Hepp 1974, Yaniv and Sade 1983, Jacobs and Potsic 1994). GT are more common in women (Rohit, Jain et al. 2003).
Presentation: tinnitus
Tinnitus is the most common presentation of GT (Larson, Reese et al. 1987, O’Leary, Shelton et al. 1991, Baguley, Irving et al. 1994, Liscak, Vladyka et al. 1998, Weissman and Hirsch 2000, Rohit, Jain et al. 2003, Tatla, Savy et al. 2003, Neto, Vuono et al. 2005, Devuyst, Defreyne et al. 2016, Daneshi, Asghari et al. 2017, Ohki and Kikuchi 2019, Lee, Lee et al. 2021, Ghate, Bhatnagar et al. 2022), and is the primary symptom in over half of cases (O’Leary, Shelton et al. 1991). The tinnitus is almost always pulsatile, but non-pulsatile tinnitus has been reported (Fukushima, Hara et al. 2018).
Presentation: hearing loss
GT is often associated with hearing loss (Larson, Reese et al. 1987, O’Leary, Shelton et al. 1991, Alshaikhly, Hamid et al. 1994, Baguley, Irving et al. 1994, Tatla, Savy et al. 2003, Neto, Vuono et al. 2005, Kumar, Andreou et al. 2014, Devuyst, Defreyne et al. 2016, Daneshi, Asghari et al. 2017, Ghate, Bhatnagar et al. 2022). Hearing loss is the second most common presenting symptom of GT, occurring in about a third of cases (O’Leary, Shelton et al. 1991). The hearing loss is usually mixed conductive and sensorineural (Daneshi, Asghari et al. 2017).
Presentation: disequilibrium
Disequilibrium is an uncommon presentation of GT, but has been reported (Liscak, Vladyka et al. 1998, Reddy 2011).
Presentation: epistaxis
Rarely, GT can present with epistaxis (Lum, Keller et al. 2001, Tatla, Savy et al. 2003).
Physical examination
A compatible clinical history should prompt examination of the external auditory canal with binocular otomicroscopy, or at least with otoscopy. The classic presentation is a red, sometimes visibly pulsatile, mass behind the eardrum.
The Figure below from Lee and Park (Lee and Park 2010) shows a red mass behind the eardrum.
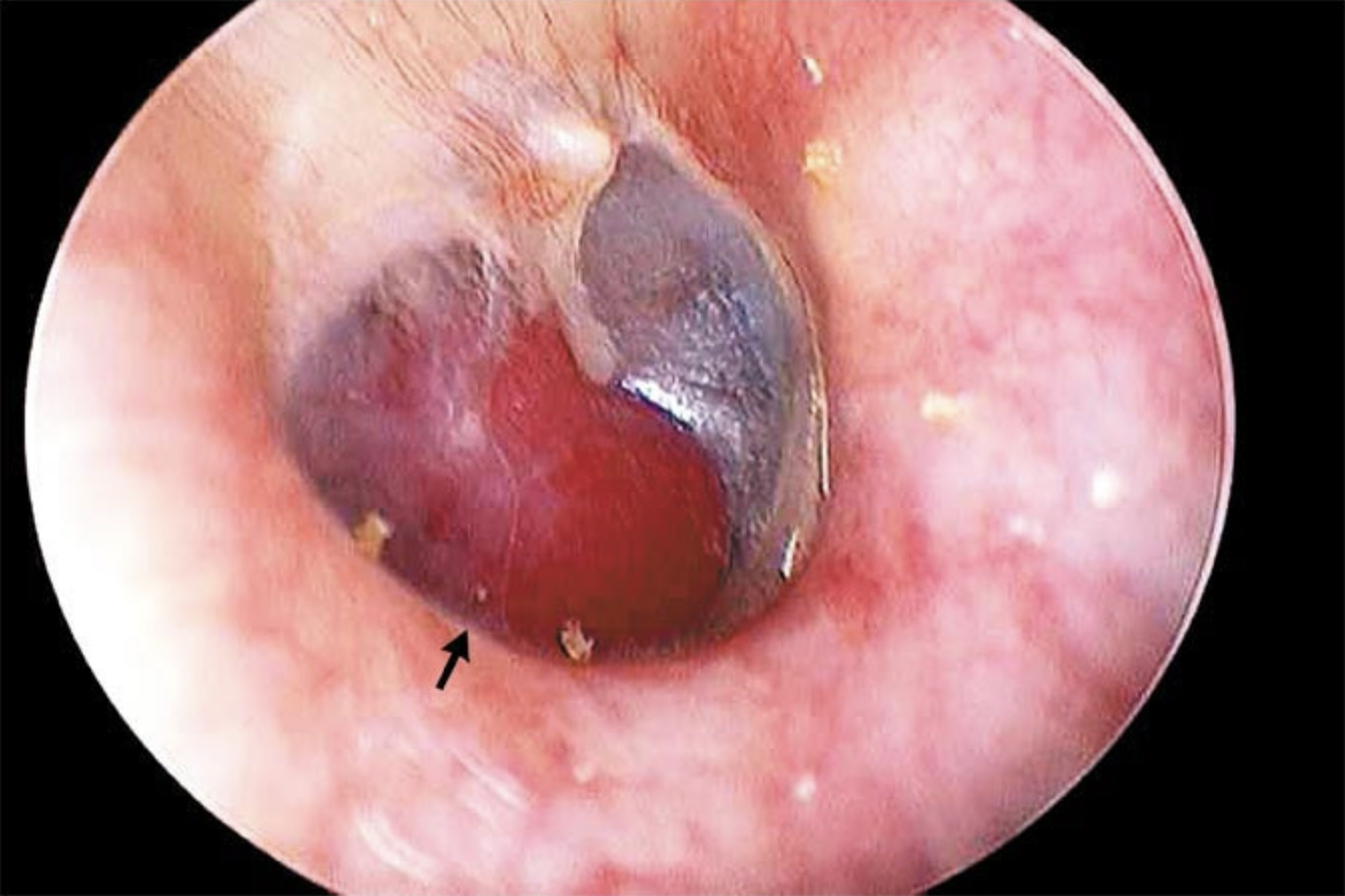
The Video below from Lee and Park (Lee and Park 2010) shows video endoscopy of GT.
Glomus tympanicum can be mimicked by other diseases
A number of other pathologies can appear similar to GT, including middle ear adenomatous tumors (Bierry, Riehm et al. 2010), extramedullary hemopoietic masses (Chen, Espinel et al. 2018), carcinoid tumor of the middle ear (Chang, Silva et al. 2022), malignant hemangioendotheioma of the temporal bone (Goldstein, Bowen et al. 1994), metastatic carcinoma of the temporal bone (Hellier, Crockard et al. 1997), promontory hemangioma (Karatas, Durucu et al. 2012), endolymphatic sac tumor (Muller, Zammit-Maempel et al. 2010), aberrant petrous carotid artery (McKiever, Carlson et al. 2014), persistent stapedial artery (Sullivan, Curtin et al. 2019), jugular bulb diverticulum (Te, Ong et al. 2021), middle ear cholesterol granuloma (Olcott and Strasnick 2017) and middle ear polyp (Shew, Bush et al. 2017).
Glomus tympanicum can mimic other diseases
GT can “transgress the tympanic membrane and appear as an inflammatory polyp in the external auditory canal” (Rohit, Jain et al. 2003).
The clinical behavior of GT can mimic Ménière’s disease (Fitzgerald 1985).
Glomus tympanicum can be comorbid with other otologic diseases
Unusually, GT can co-occur with other otologic diseases, such as cholesteatoma (Gulati 2020) or otosclerosis (Yanagisawa and Principato 1970).
Location
Some GTs arise from the tympanic nerve (Jacobson’s nerve) which traverses the middle ear, and in such cases the lesions may originate from any location along the medial wall of the middle ear (Weissman and Hirsch 1998).
Anatomical extension
In some cases GT can extend intracranially (Anand, Leonetti et al. 1993), including into the middle cranial fossa (Carlson, Sasaki et al. 1987). GT can also extend into the nasopharynx (Hirunpat, Riabroi et al. 2006) or even the cervical region (Ma, Ji et al. 2012).
Testing
Audiologic findings are well-reported in GT (Black, Berger et al. 1979, Baguley, Irving et al. 1994, Thiede, Stoll et al. 2004, Papaspyrou, Mewes et al. 2011, Medina, Prasad et al. 2014, Patnaik, Prasad et al. 2015, Devuyst, Defreyne et al. 2016, Daneshi, Asghari et al. 2017, Walker and Babu 2019). While this is interesting, diagnosis of GT does not rely on audiometry.
The role of audiometry is more important when comparing hearing at diagnosis with post-treatment outcomes.
Imaging: CT
Most investigators endorse high-resolution temporal bone CT as the imaging modality of choice in diagnosing GT (Mafee, Valvassori et al. 1983, Phelps and Lloyd 1983, Som, Reede et al. 1983).
Imaging: MRI
A few studies recognize complementary roles of CT and MRI in the diagnosis of GT (Amin and El Ameen 2013).
Imaging: angiography
Some studies report a potential role for MR angiography, digital subtraction angiography or transcranial spectral Doppler in the diagnosis of GT (De Candia, Como et al. 2002).
Treatment
Surgery was the mainstay of treatment for decades, and there is a lively debate in the literature regarding optimal surgical approaches (Cannon 1962, Smith and Shinn 1976, Farrior 1984, Sillars and Fagan 1993, Jackson 2001, Alaani, Chavda et al. 2009, Sanna, Fois et al. 2010, Chou, Huang et al. 2011, Papaspyrou, Mewes et al. 2011, Patnaik, Prasad et al. 2015, Pollak and Soni 2017, Noel and Sajjadi 2018, Ohki and Kikuchi 2019, Kaul, Filip et al. 2020, Fermi, Ferri et al. 2021).
More recently radiation therapy has become an accepted treatment modality (Konefal, Pilepich et al. 1987, Hansen and Thomsen 1988, Boyle, Shimm et al. 1990, Powell, Peters et al. 1992, Pemberton, Swindell et al. 2005, Lee, Pan et al. 2011, Kunzel, Iro et al. 2012, Liscak, Urgosik et al. 2014, Jansen, Timmers et al. 2018, Sahyouni, Mahboubi et al. 2018, Scheick, Morris et al. 2018, Fatima, Pollom et al. 2021, Kalhoro and Hashim 2023), and is often combined with surgery. As with any radiation therapy, complications include damage of healthy tissue, accelerated atherosclerosis, and subsequent increased risk of malignancy.
Embolization (sometimes followed by surgery) has been another fairly well-studied treatment modality (Boyle, Shimm et al. 1990, Tasar and Yetiser 2004, Kouzaki, Fukui et al. 2008, Sawlani, Browing et al. 2009, Devuyst, Defreyne et al. 2016), though like any embolization procedure carries a risk of stroke (Sawlani, Browing et al. 2009, Kajtazi, Manzoor et al. 2022).
Less studied treatment modalities include laser coagulation (Robinson, Grant et al. 1993, Molony, Salto-Tellez et al. 1998, Durvasula, De et al. 2005, Kouzaki, Fukui et al. 2008, Noel and Sajjadi 2018) and piezoelectric surgery (Salami, Mora et al. 2008, Salami, Dellepiane et al. 2009).
Recurrence
Recurrence of treated GT is uncommon.
A case series of 8 surgically-treated GTs reported no recurrences at up to 15 years (Cole 1979). A case series of 16 radiation-treated GTs reported no recurrences at a mean follow-up of 10.5 years (range 4 – 24 years).
One series of 17 surgically-treated cases of GT reported recurrence in 1 patient (6%) after 9 years (Rohit, Jain et al. 2003). Another series of 73 surgically-treated cases reported a recurrence rate of 5% (O’Leary, Shelton et al. 1991). One series noted persistence and/or recurrence of surgically-treated GT only in patients in whom the tumor had invaded the central nervous system (Spector and Sobol 1980).
Some series report a lower rate of recurrence with radiation-treated GT compared to surgically-treated cases (Contrera, Yong et al. 2020).
References
Alaani A, Chavda SV, Irving RM (2009) The crucial role of imaging in determining the approach to glomus tympanicum tumours. Eur Arch Otorhinolaryngol 266: 827-31. doi: 10.1007/s00405-008-0829-z
Alshaikhly A, Hamid AM, Azadeh B (1994) Glomus tympanicum chemodectoma: unusual radiological findings. J Laryngol Otol 108: 607-9. doi: 10.1017/s0022215100127586
Amin MF, El Ameen NF (2013) Diagnostic efficiency of multidetector computed tomography versus magnetic resonance imaging in differentiation of head and neck paragangliomas from other mimicking vascular lesions: comparison with histopathologic examination. Eur Arch Otorhinolaryngol 270: 1045-53. doi: 10.1007/s00405-012-2084-6
Anand VK, Leonetti JP, al-Mefty O (1993) Neurovascular considerations in surgery of glomus tumors with intracranial extensions. Laryngoscope 103: 722-8. doi: 10.1288/00005537-199307000-00003
Baguley DM, Irving RM, Hardy DG, Harada T, Moffat DA (1994) Audiological findings in glomus tumours. Br J Audiol 28: 291-7. doi: 10.3109/03005369409077313
Balatsouras DG, Eliopoulos PN, Economou CN (1992) Multiple glomus tumours. J Laryngol Otol 106: 538-43. doi: 10.1017/s0022215100120080
Bierry G, Riehm S, Marcellin L, Stierle JL, Veillon F (2010) Middle ear adenomatous tumor: a not so rare glomus tympanicum-mimicking lesion. J Neuroradiol 37: 116-21. doi: 10.1016/j.neurad.2009.05.003
Black MJ, Berger H, Tritt RA, Schloss MD (1979) Impedance audiometry: its use in the diagnosis of glomus tympanicum tumors. J Otolaryngol 8: 360-7.
Boyle JO, Shimm DS, Coulthard SW (1990) Radiation therapy for paragangliomas of the temporal bone. Laryngoscope 100: 896-901. doi: 10.1288/00005537-199008000-00018
Branica S, Sprem N, Danilovic Z, Seiwerth S (1993) Immunohistochemistry of glomus jugulare and tympanicum tumors. Acta Med Croatica 47: 123-4.
Busby DR, Hepp VE (1974) Glomus tympanicum tumor in infancy. Arch Otolaryngol 99: 377-8. doi: 10.1001/archotol.1974.00780030389013
Cannon SJ (1962) Glomus tympanicum removal by transmeatal approach. Laryngoscope 72: 193-200. doi: 10.1288/00005537-196202000-00006
Carlson RD, Sasaki CT, Friedman SI, Spencer D (1987) Glomus tympanicum tumor with middle cranial fossa extension. Otolaryngol Head Neck Surg 96: 186-9. doi: 10.1177/019459988709600212
Chang H, Silva MA, Torres AA, Weng J, de Lima Guido LP, Velez-Torres J, Gultekin SH, Brown CS, Diwanji T, Angeli SI, Benjamin C (2022) A carcinoid tumor of the middle ear masquerading as a glomus tympanicum presenting with temporal lobe hemorrhage in a 70-year-old woman: Case report and review of the literature. Neurochirurgie 68: 654-660. doi: 10.1016/j.neuchi.2022.07.008
Chen LN, Espinel A, Reilly B, Luca DC (2018) Extramedullary Hematopoiesis Presenting as Bilateral Glomus Tympanicum-First Case Report in a Pediatric Patient and With Bilateral Presentation. Pediatr Dev Pathol 21: 332-334. doi: 10.1177/1093526617704267
Chou YL, Huang BR, Wang CH (2011) En bloc surgical removal of an asymptomatic glomus tympanicum tumor. J Chin Med Assoc 74: 520-2. doi: 10.1016/j.jcma.2011.09.009
Cole JM (1979) Panel discussion: glomus jugulare tumors of the temporal bone. Radiation of glomus tumors of the temporal bone. Laryngoscope 89: 1623-7. doi: 10.1002/lary.5540891013
Contrera KJ, Yong V, Reddy CA, Liu SW, Lorenz RR (2020) Recurrence and Progression of Head and Neck Paragangliomas after Treatment. Otolaryngol Head Neck Surg 162: 504-511. doi: 10.1177/0194599820902702
Daneshi A, Asghari A, Mohebbi S, Farhadi M, Farahani F, Mohseni M (2017) Total Endoscopic Approach in Glomus Tympanicum Surgery. Iran J Otorhinolaryngol 29: 305-311.
De Candia A, Como G, Passon P, Pedace E, Bazzocchi M (2002) Sonographic findings in glomus tympanicum tumor. J Clin Ultrasound 30: 236-40. doi: 10.1002/jcu.10058
Devuyst L, Defreyne L, Praet M, Geukens S, Dhooge I (2016) Treatment of glomus tympanicum tumors by preoperative embolization and total surgical resection. Am J Otolaryngol 37: 544-551. doi: 10.1016/j.amjoto.2016.08.011
Durvasula VS, De R, Baguley DM, Moffat DA (2005) Laser excision of glomus tympanicum tumours: long-term results. Eur Arch Otorhinolaryngol 262: 325-7. doi: 10.1007/s00405-004-0822-0
Farrior JB (1984) Anterior hypotympanic approach for glomus tumor of the infratemporal fossa. Laryngoscope 94: 1016-21. doi: 10.1288/00005537-198408000-00004
Fatima N, Pollom E, Soltys S, Chang SD, Meola A (2021) Stereotactic radiosurgery for head and neck paragangliomas: a systematic review and meta-analysis. Neurosurg Rev 44: 741-752. doi: 10.1007/s10143-020-01292-5
Fermi M, Ferri G, Bayoumi Ebaied T, Alicandri-Ciufelli M, Bonali M, Badr El-Dine M, Presutti L (2021) Transcanal Endoscopic Management of Glomus Tympanicum: Multicentric Case Series. Otol Neurotol 42: 312-318. doi: 10.1097/MAO.0000000000002929
Fitzgerald DC (1985) Glomus tympanicum presenting as Meniere’s disease. Ear Nose Throat J 64: 68.
Fountarlis AL, Hajiioannou J, Lachanas V, Tsitiridis I, Saratziotis A, Alagianni A, Skoulakis C (2022) Endoscopic Management of Glomus Tympanicum Tumor: Report of Three Cases and Review of the Literature. J Audiol Otol. doi: 10.7874/jao.2022.00276
Fukushima H, Hara H, Paparella MM, Oktay MF, Schachern PA, Cureoglu S (2018) Bilateral glomus tympanicum tumors: Human temporalbone study. Clin Pract 8: 1035. doi: 10.4081/cp.2018.1035
Ghate G, Bhatnagar A, Mukhtar S (2022) Post-Embolization Excision of Glomus Tympanicum: A Case Report. Cureus 14: e21414. doi: 10.7759/cureus.21414
Goldstein WS, Bowen BC, Balkany T (1994) Malignant hemangioendothelioma of the temporal bone masquerading as glomus tympanicum. Ann Otol Rhinol Laryngol 103: 156-9. doi: 10.1177/000348949410300213
Gulati K (2020) Unusual presentation of a large glomus tympanicum with a coexisting cholesteatoma. Clin Case Rep 8: 2429-2432. doi: 10.1002/ccr3.3175
Hansen HS, Thomsen KA (1988) Radiotherapy in glomus tumours (paragangliomas). A 25 year-review. Acta Otolaryngol Suppl 449: 151-4. doi: 10.3109/00016488809106399
Hellier WP, Crockard HA, Cheesman AD (1997) Metastatic carcinoma of the temporal bone presenting as glomus jugulare and glomus tympanicum tumours: a description of two cases. J Laryngol Otol 111: 963-6. doi: 10.1017/s0022215100139088
Hirunpat S, Riabroi K, Dechsukhum C, Atchariyasathian V, Tanomkiat W (2006) Nasopharyngeal extension of glomus tympanicum: an unusual clinical and imaging manifestation. AJNR Am J Neuroradiol 27: 1820-2.
Jackson CG (2001) Glomus tympanicum and glomus jugulare tumors. Otolaryngol Clin North Am 34: 941-70, vii. doi: 10.1016/s0030-6665(05)70356-x
Jacobs IN, Potsic WP (1994) Glomus tympanicum in infancy. Arch Otolaryngol Head Neck Surg 120: 203-5. doi: 10.1001/archotol.1994.01880260073013
Jansen TTG, Timmers H, Marres HAM, Kaanders J, Kunst HPM (2018) Results of a systematic literature review of treatment modalities for jugulotympanic paraganglioma, stratified per Fisch class. Clin Otolaryngol 43: 652-661. doi: 10.1111/coa.13046
Kajtazi NI, Manzoor MU, Ghamdi JA, Zahrani HA, Suwaidan FA, Qahtani SA, Bafaquh M (2022) Right cerebellar stroke with a right vertebral artery occlusion following an embolization of the right glomus tympanicum tumor: Case report with literature review. J Cerebrovasc Endovasc Neurosurg 24: 386-392. doi: 10.7461/jcen.2022.E2021.11.002
Kalhoro A, Hashim ASM (2023) Glomus jugulare tumors treatment by gamma knife radiosurgery: A single center study. Pak J Med Sci 39: 46-49. doi: 10.12669/pjms.39.1.6590
Karatas E, Durucu C, Baglam T (2012) Promontory hemangioma mimics glomus tympanicum in the middle ear (promontory hemangioma). Eur Rev Med Pharmacol Sci 16 Suppl 4: 103-5.
Kaul VF, Filip P, Schwam ZG, Wanna GB (2020) Nuances in transcanal endoscopic surgical technique for glomus tympanicum tumors. Am J Otolaryngol 41: 102562. doi: 10.1016/j.amjoto.2020.102562
Konefal JB, Pilepich MV, Spector GJ, Perez CA (1987) Radiation therapy in the treatment of chemodectomas. Laryngoscope 97: 1331-5. doi: 10.1288/00005537-198711000-00016
Kouzaki H, Fukui J, Shimizu T (2008) Management of a catecholamine-secreting tympanicum glomus tumour: case report. J Laryngol Otol 122: 1377-80. doi: 10.1017/S0022215108001801
Kumar G, Andreou Z, Virk JS, Owa A (2014) Unusual presentation of glomus tympanicum tumour: New bone formation in the middle ear. World J Clin Cases 2: 463-5. doi: 10.12998/wjcc.v2.i9.463
Kunzel J, Iro H, Hornung J, Koch M, Brase C, Klautke G, Zenk J (2012) Function-preserving therapy for jugulotympanic paragangliomas: a retrospective analysis from 2000 to 2010. Laryngoscope 122: 1545-51. doi: 10.1002/lary.23268
Larson TC, 3rd, Reese DF, Baker HL, Jr., McDonald TJ (1987) Glomus tympanicum chemodectomas: radiographic and clinical characteristics. Radiology 163: 801-6. doi: 10.1148/radiology.163.3.3033738
Lee CC, Pan DH, Wu JC, Chung WY, Wu HM, Yang HC, Liu KD, Guo WY, Shih YH (2011) Gamma knife radiosurgery for glomus jugulare and tympanicum. Stereotact Funct Neurosurg 89: 291-8. doi: 10.1159/000328890
Lee CK, Park KH (2010) Images in clinical medicine. Glomus tympanicum. N Engl J Med 362: e66. doi: 10.1056/NEJMicm0907680
Lee SJ, Lee SY, An GS, Lee K, Choi BY, Koo JW, Song JJ (2021) Treatment Outcomes of Patients with Glomus Tympanicum Tumors Presenting with Pulsatile Tinnitus. J Clin Med 10. doi: 10.3390/jcm10112348
Liscak R, Urgosik D, Chytka T, Simonova G, Novotny J, Jr., Vymazal J, Guseynova K, Vladyka V (2014) Leksell Gamma Knife radiosurgery of the jugulotympanic glomus tumor: long-term results. J Neurosurg 121 Suppl: 198-202. doi: 10.3171/2014.7.GKS14923
Liscak R, Vladyka V, Simonova G, Vymazal J, Janouskova L (1998) Leksell gamma knife radiosurgery of the tumor glomus jugulare and tympanicum. Stereotact Funct Neurosurg 70 Suppl 1: 152-60. doi: 10.1159/000056417
Lum C, Keller AM, Kassel E, Blend R, Waldron J, Rutka J (2001) Unusual eustachian tube mass: glomus tympanicum. AJNR Am J Neuroradiol 22: 508-9.
Ma CY, Ji T, Wu YQ, Ow A (2012) A jugulotympanic paraganglioma with craniocervical extension. Int J Oral Maxillofac Surg 41: 221-4. doi: 10.1016/j.ijom.2011.10.020
Mafee MF, Raofi B, Kumar A, Muscato C (2000) Glomus faciale, glomus jugulare, glomus tympanicum, glomus vagale, carotid body tumors, and simulating lesions. Role of MR imaging. Radiol Clin North Am 38: 1059-76. doi: 10.1016/s0033-8389(05)70221-9
Mafee MF, Valvassori GE, Shugar MA, Yannias DA, Dobben GD (1983) High resolution and dynamic sequential computed tomography. Use in the evaluation of glomus complex tumors. Arch Otolaryngol 109: 691-6. doi: 10.1001/archotol.1983.00800240057011
McKiever ME, Carlson ML, Neff BA (2014) Aberrant petrous carotid artery masquerading as a glomus tympanicum. Otol Neurotol 35: e228-30. doi: 10.1097/MAO.0000000000000275
Medina M, Prasad SC, Patnaik U, Lauda L, Di Lella F, De Donato G, Russo A, Sanna M (2014) The effects of tympanomastoid paragangliomas on hearing and the audiological outcomes after surgery over a long-term follow-up. Audiol Neurootol 19: 342-50. doi: 10.1159/000362617
Molony NC, Salto-Tellez M, Grant WE (1998) KTP laser assisted excision of glomus tympanicum. J Laryngol Otol 112: 956-8. doi: 10.1017/s0022215100142173
Muller M, Zammit-Maempel I, Hill J, Wilkins B (2010) An unusual middle-ear mass. J Laryngol Otol 124: 108-10. doi: 10.1017/S0022215109990442
Neto ME, Vuono IM, Souza LR, Testa JR, Pizarro GU, Barros F (2005) Tympanic paragangliomas: case reports. Braz J Otorhinolaryngol 71: 97-100. doi: 10.1016/s1808-8694(15)31293-3
Noel JE, Sajjadi H (2018) KTP-laser-assisted endoscopic management of glomus tympanicum tumors: A case series. Ear Nose Throat J 97: 399-402. doi: 10.1177/014556131809701209
O’Leary MJ, Shelton C, Giddings NA, Kwartler J, Brackmann DE (1991) Glomus tympanicum tumors: a clinical perspective. Laryngoscope 101: 1038-43. doi: 10.1288/00005537-199110000-00002
Ohki M, Kikuchi S (2019) A Small Glomus Tympanicum Tumor Resected by Minimally Invasive Transcanal Endoscopic Approach. Case Rep Otolaryngol 2019: 5780161. doi: 10.1155/2019/5780161
Olcott C, Strasnick B (2017) A blue middle ear mass: Cholesterol granuloma mimicking a glomus tumor and endolymphatic sac tumor. Am J Otolaryngol 38: 100-102. doi: 10.1016/j.amjoto.2016.09.013
Papaspyrou K, Mewes T, Toth M, Schmidtmann I, Amedee RG, Mann WJ (2011) Hearing results after hypotympanotomy for glomus tympanicum tumors. Otol Neurotol 32: 291-6. doi: 10.1097/MAO.0b013e3182001edb
Patnaik U, Prasad SC, Medina M, Al-Qahtani M, D’Orazio F, Falcioni M, Piccirillo E, Russo A, Sanna M (2015) Long term surgical and hearing outcomes in the management of tympanomastoid paragangliomas. Am J Otolaryngol 36: 382-9. doi: 10.1016/j.amjoto.2015.01.006
Pemberton LS, Swindell R, Sykes AJ (2005) Radical radiotherapy alone for glomus jugulare and tympanicum tumours. Oncol Rep 14: 1631-3.
Phelps PD, Lloyd GA (1983) Glomus tympanicum tumours: demonstration by high resolution C.T. Clin Otolaryngol Allied Sci 8: 15-20. doi: 10.1111/j.1365-2273.1983.tb01666.x
Pollak N, Soni RS (2017) Endoscopic excision of a tympanic paraganglioma: Training the next generation of ear surgeons. World J Otorhinolaryngol Head Neck Surg 3: 160-162. doi: 10.1016/j.wjorl.2017.08.002
Powell S, Peters N, Harmer C (1992) Chemodectoma of the head and neck: results of treatment in 84 patients. Int J Radiat Oncol Biol Phys 22: 919-24. doi: 10.1016/0360-3016(92)90788-j
Reddy R (2011) An unusual cause of vertigo and syncope: a case report. Hawaii Med J 70: 16-7.
Robinson PJ, Grant HR, Bown SG (1993) NdYAG laser treatment of a glomus tympanicum tumour. J Laryngol Otol 107: 236-7. doi: 10.1017/s0022215100122728
Rohit, Jain Y, Caruso A, Russo A, Sanna M (2003) Glomus tympanicum tumour: an alternative surgical technique. J Laryngol Otol 117: 462-6. doi: 10.1258/002221503321892307
Sahyouni R, Mahboubi H, Moshtaghi O, Goshtasbi K, Sahyouni S, Lin HW, Djalilian HR (2018) Radiosurgery of Glomus Tumors of Temporal Bone: a Meta-analysis. Otol Neurotol 39: 488-493. doi: 10.1097/MAO.0000000000001737
Salami A, Dellepiane M, Proto E, Mora R (2009) Piezosurgery in otologic surgery: four years of experience. Otolaryngol Head Neck Surg 140: 412-8. doi: 10.1016/j.otohns.2008.11.013
Salami A, Mora R, Dellepiane M (2008) Piezosurgery in the exeresis of glomus tympanicum tumours. Eur Arch Otorhinolaryngol 265: 1035-8. doi: 10.1007/s00405-007-0567-7
Sanna M, Fois P, Pasanisi E, Russo A, Bacciu A (2010) Middle ear and mastoid glomus tumors (glomus tympanicum): an algorithm for the surgical management. Auris Nasus Larynx 37: 661-8. doi: 10.1016/j.anl.2010.03.006
Sawlani V, Browing S, Sawhney IM, Redfern R (2009) Posterior circulation stroke following embolization of glomus tympanicum?relevance of anatomy and anastomoses of ascending pharyngeal artery. A case report. Interv Neuroradiol 15: 229-36. doi: 10.1177/159101990901500216
Scheick SM, Morris CG, Amdur RJ, Bova FJ, Friedman WA, Mendenhall WM (2018) Long-term Outcomes After Radiosurgery for Temporal Bone Paragangliomas. Am J Clin Oncol 41: 223-226. doi: 10.1097/COC.0000000000000255
Shew M, Bush J, Tawfik O, Ator G (2017) Middle Ear Aural Polyp Mimicking Glomus Tympanicum in a Male Adolescent. Otol Neurotol 38: e211-e213. doi: 10.1097/MAO.0000000000001470
Sillars HA, Fagan PA (1993) The management of multiple paraganglioma of the head and neck. J Laryngol Otol 107: 538-42. doi: 10.1017/s0022215100123643
Smith MF, Shinn JB (1976) Glomus tympanicum–excision by radical mastoidectomy exposure with autograft reconstruction. Laryngoscope 86: 431-5. doi: 10.1288/00005537-197603000-00012
Snitzer JL, Sheeler LR, Bravo EL, Thacker HL, Lavertu P (1995) A carotid body and glomus jugulare paraganglioma secreting norepinephrine. Endocr Pract 1: 82-5. doi: 10.4158/EP.1.2.82
Som PM, Reede DL, Bergeron RT, Parisier SC, Shugar JM, Cohen NL (1983) Computed tomography of glomus tympanicum tumors. J Comput Assist Tomogr 7: 14-7. doi: 10.1097/00004728-198302000-00003
Spector GJ, Sobol S (1980) Surgery for glomus tumors at the skull base. Otolaryngol Head Neck Surg (1979) 88: 524-30. doi: 10.1177/019459988008800503
Sullivan AM, Curtin HD, Moonis G (2019) Arterial Anomalies of the Middle Ear: A Pictorial Review with Clinical-Embryologic and Imaging Correlation. Neuroimaging Clin N Am 29: 93-102. doi: 10.1016/j.nic.2018.09.010
Sweeney AD, Carlson ML, Wanna GB, Bennett ML (2015) Glomus tympanicum tumors. Otolaryngol Clin North Am 48: 293-304. doi: 10.1016/j.otc.2014.12.004
Tasar M, Yetiser S (2004) Glomus tumors: therapeutic role of selective embolization. J Craniofac Surg 15: 497-505. doi: 10.1097/00001665-200405000-00031
Tatla T, Savy LE, Wareing MJ (2003) Epistaxis as a rare presenting feature of glomus tympanicum. J Laryngol Otol 117: 577-9. doi: 10.1258/002221503322113085
Te BC, Ong KP, Zainon IH (2021) A Rare Cause of Red Tympanic Membrane: Jugular Bulb Diverticulum. Ear Nose Throat J: 1455613211031384. doi: 10.1177/01455613211031384
Thiede O, Stoll W, Schmal F (2004) Clinical and experimental investigations of spontaneous impedance changes of the middle ear. Ann Otol Rhinol Laryngol 113: 577-81. doi: 10.1177/000348940411300712
Walker DD, Babu S (2019) Temporal Bone Paraganglioma: Hearing Outcomes and Rehabilitation. J Neurol Surg B Skull Base 80: 209-213. doi: 10.1055/s-0039-1679890
Weissman JL, Hirsch BE (1998) Beyond the promontory: the multifocal origin of glomus tympanicum tumors. AJNR Am J Neuroradiol 19: 119-22.
Weissman JL, Hirsch BE (2000) Imaging of tinnitus: a review. Radiology 216: 342-9. doi: 10.1148/radiology.216.2.r00au45342
Wieser ME, Gilley DR, May JG, Rivera AL (2022) A rare case of a middle ear glomangioma. SAGE Open Med Case Rep 10: 2050313X211070520. doi: 10.1177/2050313X211070520
Yanagisawa E, Principato JJ (1970) Glomus tympanicum tumor in an otosclerotic ear. Arch Otolaryngol 91: 299-301. doi: 10.1001/archotol.1970.00770040405017
Yaniv E, Sade J (1983) Glomus tympanicum tumors in a child. Int J Pediatr Otorhinolaryngol 5: 93-7. doi: 10.1016/s0165-5876(83)80011-1
![]()