By Marcello Cherchi, MD PhD
For patients
Here are answers to some of the most common questions about computed tomography (CT).
|
What is this test? |
Computed tomography (CT) is a way of taking a special picture of the inside of the body. |
|
What is this test looking for? |
This test is good at taking pictures of bones. It is not so good for taking pictures of soft parts of the body. |
|
Is this test experimental or investigational? |
This test is approved by the Food and Drug Administration. It is neither experimental nor investigational. |
|
What happens during this test? |
During this test you are usually lying on a table that slowly slides in and out of a machine. |
|
Is this test uncomfortable? |
The test does not hurt. |
|
How long does this test take? |
The test can take anywhere from a few minutes to half an hour, depending on the pictures being taken. |
|
Do I have to prepare for this test? |
You should not be wearing any metal objects during this test. You should tell the radiology doctor if you are pregnant. There are otherwise no specific preparations for this test. |
|
Are there any special instructions for what to do after the test? |
There are no special instructions for what to do after this test. |
For clinicians
Overview
Computed tomography (CT) is an excellent imaging modality for studying the anatomy and structure of bone. This can be especially helpful for certain disorders in otoneurology and neuro-otology. In otoneurology a common protocol is to check a temporal bone CT without contrast. The test is subject to artifact from metals. CT is based on the ionizing radiation of X‑rays, which entails some risk of tissue damage and increases the risk of malignancy, and these risks should be considered when ordering a CT of any type.
Introduction
There are several diseases in otoneurology for which imaging of bone is helpful. Computed tomography (CT) is currently the diagnostic modality of choice for this.
Equipment needed
CT scanners are usually housed in a hospital radiology service. Some clinics also have CT scanners.
How to perform the test
The specific protocol for a CT depends on the differential diagnosis being considered.
In otoneurology the usual anatomical areas of interest are the vestibular structures in the temporal bone. In some cases, intravenous contrast may be appropriate.
One of the more common otoneurological reasons for checking a CT is to assess for superior semicircular canal dehiscence (SSCD). The best studied imaging modality to evaluate for SSCD is a temporal bone CT without contrast. The collimation cuts should be 0.6 mm or better. Depending on the radiology service’s experience, it may be helpful to protocol the study with reconstructions in Stenver’s and Pöschl’s projections.
Pöschl’s projection (Pöschl 1943), named after Max Pöschl (1909-1990), is also referred to as the axiopetrosal plane or axial pyramidal plane, because it is perpendicular to the petrous pyramid. The plane of this projection runs from anterolateral to posteromedial, which is in the same plane as the superior semicircular canal.
Stenver’s projection (Stenvers 1916, 1917), named after Hendrik Willem Stenvers (1889-1973). The plane of this projection runs from anteromedial to posterolateral. Stenver’s projection acquires images through the semicircular canal “end on.”
These planes can be imagined by thinking of the so-called RALP-LARP planes. “RALP” refers to the fact that planes of the Right Anterior semicircular canal and the Left Posterior canal are parallel. “LARP” refers to the fact that the Left Anterior semicircular canal and the Right Posterior semicircular canal are parallel. These are depicted in the Figure below from Aw and colleagues (Aw et al. 2010).
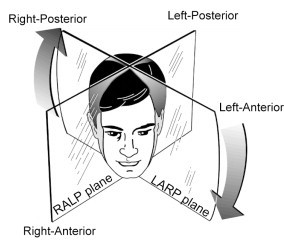
For the right superior semicircular canal, Stenver’s view corresponds to a projection through the LARP plane, while Pöschl’s view corresponds to a projection through the RALP plane.
For the left superior semicircular canal, Stenver’s view corresponds to a projection through the RALP plane, while Pöschl’s view corresponds to a projection through the LARP plane.
Thus, the coronal plane, Stenver’s plane and Pöschl’s plane provide three different views of the superior semicircular canal. The Figure below, from Duman and Dogan (Duman and Dogan 2020), juxtaposes three panels containing each view taken of a patient with superior SCD.
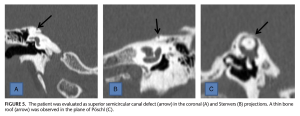
Performing a temporal bone CT entails exposure to a significant amount of ionizing radiation, so there is interest in other imaging modalities that could avoid this risk. MRI does not image bone well, but studies are beginning to explore whether high resolution MRI has utility in the diagnosis of SSCD (Beyazal Celiker et al. 2018).
What this test assesses
CT is an excellent tool for evaluating bony structures.
CT is less useful for evaluating soft tissues (such as neural structures).
How to interpret the test results
CT is interpreted by a radiologist.
Limitations
CT is a relatively quick test (minutes), but it is still necessary for the patient to remain still during that period in order to obtain good quality images.
CT is subject to metal artifact from implanted devices.
Contraindications
There are no firm contraindications to undergoing CT. However, CT is based on the ionizing radiation of X‑rays, which entails some risk of tissue damage, and also increases the risk of malignancy.
Pregnancy is a relative contraindication to undergoing CT. If absolutely necessary, the mother’s abdomen and pelvis can be shielded in order to limit the fetus’ exposure to radiation.
When is the test indicated
The indication for imaging depends on the differential diagnosis under consideration.
Diseases that may be diagnosed by this test
CT is a very useful tool to study the anatomical structure of bone. It can be helpful in the diagnosis of several diseases in otoneurology, such as labyrinthine ossification, cholesteatoma, semicircular canal dehiscence, otosclerosis, Paget’s disease of bone, fibrous dysplasia, temporal bone fracture, congenital otologic malformations (large vestibular aqueduct, large cochlear aqueduct, Mondini dysplasia, Pendred syndrome, Usher syndrome), and others.
References
Aw ST, Todd MJ, Michael Halmagyi G (2010) Chapter 12 – Head impulse testing: angular vestibulo-ocular reflex (VOR). Handbook of Clinical Neurophysiology, vol 9. Elsevier, pp 150-164
Beyazal Celiker F, Ozgur A, Celiker M, Beyazal M, Turan A, Terzi S, Inecikli MF (2018) The Efficacy of Magnetic Resonance Imaging for the Diagnosis of Superior Semicircular Canal Dehiscence. J Int Adv Otol 14: 68-71. doi: 10.5152/iao.2017.4103
Duman IS, Dogan SN (2020) Contribution of Reformatted Multislice Temporal Computed Tomography Images in the Planes of Stenvers and Poschl to the Diagnosis of Superior Semicircular Canal Dehiscence. J Comput Assist Tomogr 44: 53-58. doi: 10.1097/RCT.0000000000000957
Pöschl M (1943) Der tomographische Querschnitt durch das Felsenbein [The tomographic cross-section through the petrous bone]. Forschrtschritte auf der Gebiete des Röntgenstrahlen [Advances in Radiology] 68: 174-179.
Stenvers HW (1916) The clinical significance of radiographs of the orbital region. Archives of Radiology and Electrotherapy 20: 411-417.
Stenvers HW (1917) Roentgenology of the os petrosum. Archives of Radiology and Electrotherapy 22: 97-112.
![]()