By Marcello Cherchi, MD PhD
For patients
Here are answers to some of the most common questions about ocular vestibular evoked myogenic potentials testing.
|
What is this test? |
The test of ocular vestibular evoked myogenic potentials (oVEMPs) assesses part of the balance system of the inner ear. |
|
What is this test looking for? |
This test looks for changes in tone of some of the muscles around the eyes in response to sounds. |
|
Is this test experimental or investigational? |
This test is approved by the Food and Drug Administration. It is neither experimental nor investigational. |
|
What happens during this test? |
During this test the audiologist or technician usually has you sit in a chair and keep the head level but direct your eyes upwards. They place an earbud insert earphone in your ear and apply electrodes on your face and neck. You hear a series of loud tones. This is performed once in each ear. |
|
Is this test uncomfortable? |
The test is not uncomfortable. |
|
How long does this test take? |
The test takes about 30 minutes. |
|
Do I have to prepare for this test? |
If you have ear wax, this should be removed before the test. There are otherwise no specific preparations for this test. |
|
Are there any special instructions for what to do after the test? |
There are no special instructions for what to do after this test. |
For clinicians
Overview
Ocular vestibular evoked myogenic potentials (oVEMPs) are reflex myogenic potentials usually elicited by vibration-induced stimulation of the utricle. The myogenic response is measured from the inferior oblique muscle by surface electrodes placed below the eye contralateral to the acoustic stimulus. The test assesses the pathway from the utricle, through the superior division of the vestibular nerve, to the medial vestibular nucleus, through the contralateral medial longitudinal fasciculus to the oculomotor nucleus, to the inferior oblique muscle. It is reasonable to check oVEMPs in some patients with the symptom of disequilibrium, and some patients with certain auditory symptoms (such as hyperacusis, pulsatile tinnitus, or autophony).
Introduction
Ocular vestibular evoked myogenic potentials (oVEMPs) are a reflex change in muscle tone of the inferior oblique in response to a vestibular signal arising from acoustic stimulation (less commonly from bone vibration stimulus) of the utricle.
Physiology and neuroanatomy
The oVEMP response is thought to originate in the utricle. The utricle is one of the two otolith organs in each labyrinth, as shown in the Figure below.
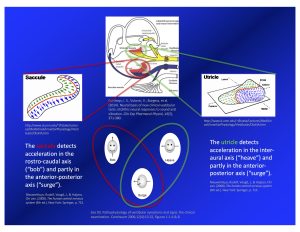
The dispositions of the utricles in the skull is depicted in the Figure below, from Miller (Miller 1962).
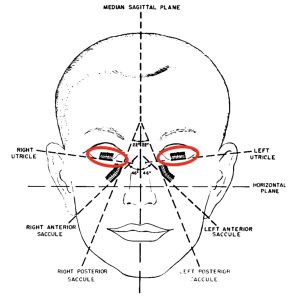
The utricle detects linear acceleration primarily along the inter-aural axis (“heave”), and less along the anterior-posterior axis (“surge”). Stimulation of the utricle elicits several responses, including the following oligosynaptic pathway:
- First-order neuron
- Receptor in the utricle
- Cell body resides in the vestibular (Scarpa’s) ganglion
- Projects axons through the superior division of the vestibular nerve
- Synapses in the medial vestibular nucleus
- Second-order neuron
- Cell body resides in the medial vestibular nucleus
- The projection decussates and ascends through the contralateral medial longitudinal fasciculus to the oculomotor nucleus
- These projections synapse in the oculomotor nucleus
- Third-order neuron
- Cell body resides in the oculomotor nucleus
- Projects to the inferior oblique muscle and synapses at the neuromuscular junction
This pathway is schematically depicted in the Figure below, from Fife and colleagues (Fife et al. 2017).
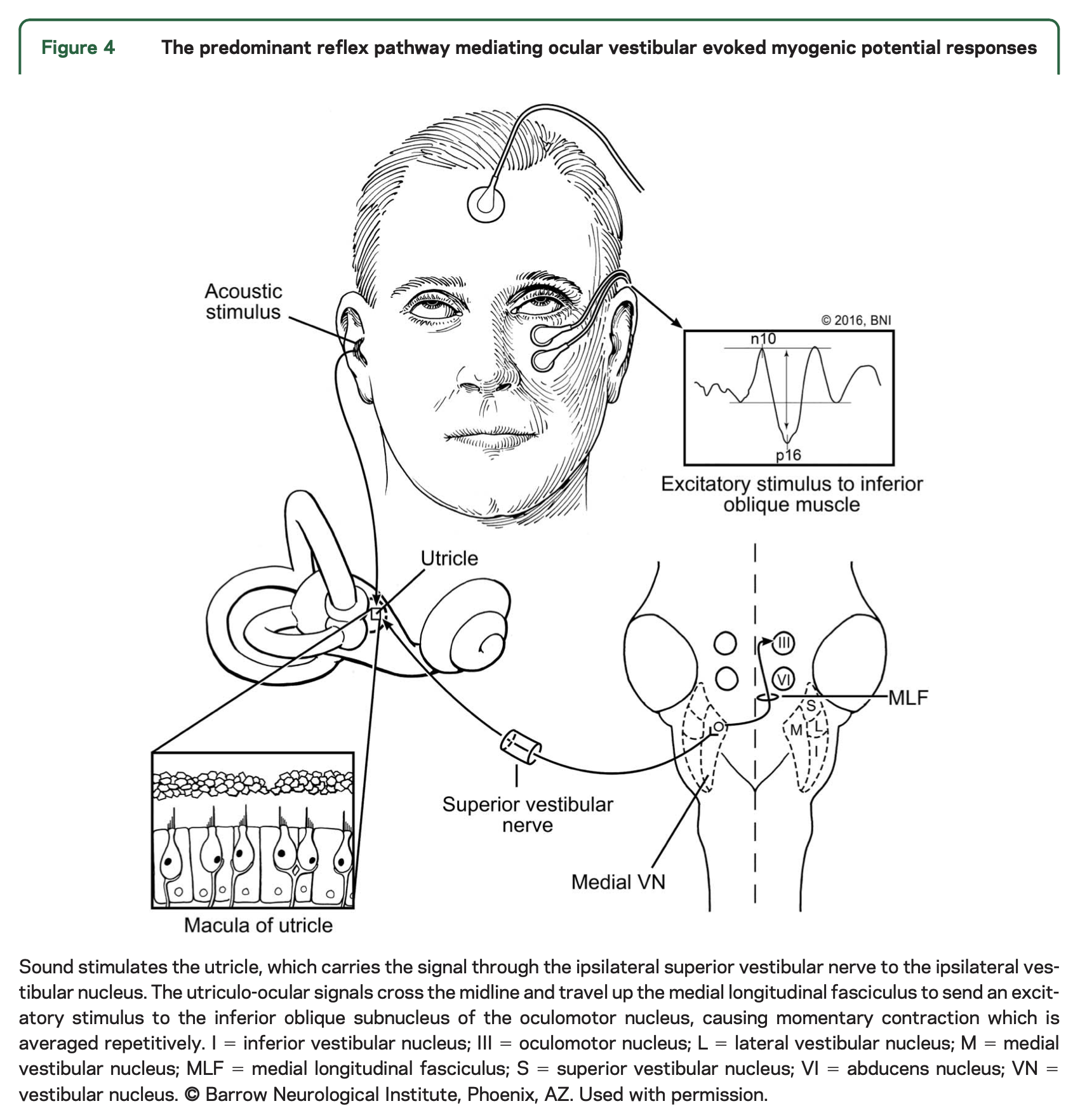
A lesion anywhere along this pathway may affect oVEMP responses.
Equipment needed
Depending on the clinical scenario, the stimulus generator can be acoustic (through earbud insert earphones) or vibratory (from a bone vibrator). When feasible it is desirable to use an acoustic stimulus because it is easier to stimulate one ear at a time. Using a bone vibrator is more likely to deliver a vibratory stimulus to both labyrinths.
The equipment for measuring myogenic responses from surface electrodes is similar to other evoked myogenic potential machines. The software is customized to the timing, amplitude and response-averaging parameters relevant for oVEMPs.
How to perform the test
If the oVEMP is to be performed using acoustic stimuli, then make sure there is no occlusion of the external auditory canal (such as from cerumen), and make sure that there is no conductive hearing loss.
The amplitude of the oVEMP signal is small (since the muscle is so small). Similar to other VEMPs, the responses of oVEMPs will be more robust if the muscle is contracted (beyond its tonic state). This is accomplished by having the patient keep the head in a neutral position while directing their gaze upward at a fixed target; this activates the inferior oblique muscles. The patient maintains this direction of gaze during the collection of responses. Since the level of activation of the inferior oblique muscle influences the magnitude of the oVEMP response (Cengiz et al. 2023; Govender et al. 2009; Kantner and Gurkov 2014), the laboratory should make an effort to standardize the upward gaze angle.
The acoustic stimulus (which can be either a tone burst or a click) is generated by a for-purpose stimulator. The most common protocol is to use a tone burst of 500 Hz at 95 dB. The myogenic potentials are collected from repeated cycles and response averaging is performed.
The usual montage for oVEMP is (Dlugaiczyk 2020):
- Active electrode is placed on the infraorbital rim in line with the pupil (the skin covering the inferior oblique).
- Reference electrode is placed 1 – 2 cm below the active electrode.
- Ground electrode is placed on the chin or sternum.
What this test assesses
Ocular vestibular evoked myogenic potentials (oVEMPs) assess the integrity of the neuroanatomical pathway described above from the utricle to the contralateral inferior oblique muscle, and is sensitive to lesions anywhere along that pathway.
How to interpret the test results
Ocular vestibular evoked myogenic potentials are usually much more robust contralateral to the stimulated ear, whereas they are usually absent or much smaller ipsilaterally. This is shown in the Figure below, from Dlugaiczyk (Dlugaiczyk 2020).
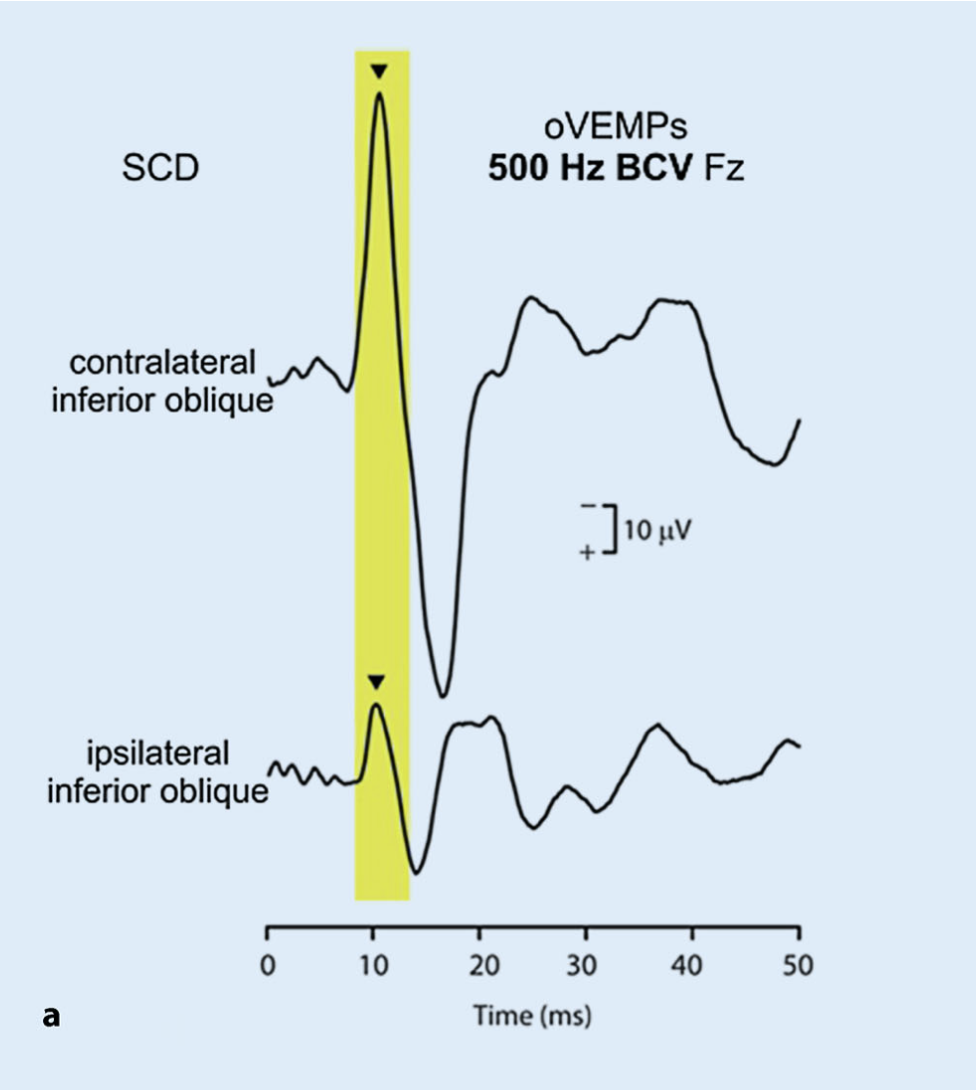
A normal ocular vestibular evoked myogenic potential response has an expected latency (n10). Normative ranges for the amplitude have been debated.
From the absolute amplitudes, asymmetry can be calculated using Jongkees formula (Jongkees et al. 1962). The upper normal limit of asymmetry has also been a matter of debate, ranging from a low of 34% – 35.3% (Chihara et al. 2007; Piker et al. 2011) to a high of 41.8% – 43% (Murnane et al. 2011; Park et al. 2010).
Clinically we find the asymmetry between the two ears to be more informative than the absolute amplitudes.
The effect of age on oVEMP responses
Age has been shown to affect oVEMP responses.
- Agrawal and colleagues studied oVEMPs and reported that advancing age negatively correlates with amplitudes (Agrawal et al. 2012).
- Sing and Firdose studied oVEMPs and reported that advancing age positively correlates with latencies, negatively correlates with amplitues, and negatively correlates with response rates overall (Singh and Firdose 2021).
In summary, there is evidence that advancing age causes an increase in latencies, an increase in thresholds, a decrease in amplitude and a decrease in overall oVEMP responses. Thus, in an older individual, symmetrically absent oVEMPs are generally not diagnostically meaningful.
Limitations
Vestibular evoked myogenic potentials that use acoustic stimuli rely on the integrity of the middle ear to transmit the vibrations from sound to the labyrinth. Thus, conductive hearing loss can interfere with oVEMP results. For this reason it is desirable to have a recent audiogram when performing and interpreting acoustically-elicited oVEMPs. In patients with conductive hearing loss, the audiologist or technician may switch to using a bone vibrator for the stimulus.
Contraindications
Acoustically-elicited VEMPs generally use earbud insert earphones, which is relatively contraindicated in patients with external ear problems such as otitis externa or recent injury.
Pitfalls
Keep in mind that non-vestibular lesions can result in abnormal VEMPs. For example, a patient with ocular myasthenia gravis will have weak extraocular muscles (and thus a weak or absent oVEMP) even though the peripheral vestibular system is intact.
When evaluating an asymmetry in ocular vestibular evoked myogenic potentials, keep in mind that the side with the smaller response may be too weak, or the side with the larger response may be too strong.
- In most cases, the stimulated ear opposite the smaller oVEMP response will be the side with pathology (remember that the oVEMP response is measured in the eye contralateral to the ear that received the acoustic stimulus).
- However, there are some cases in which the stimulated ear (opposite the eye from which the oVEMP is measured) with the larger amplitude oVEMP is the side with pathology. This usually occurs in third window phenomena such as semicircular canal dehiscence (SCD). In the case of SCD, there may also be low oVEMP thresholds, and audiometry may show conductive hyperacusis.
The earbud insert earphones can burn out. Improperly cleaned skin beneath electrodes can lead to high electrical impedance and interfere with measurement of myogenic responses. There is sometimes artifact from electrical interference.
When is the test indicated
Ocular vestibular evoked myogenic potentials comprise a reasonable tool for testing utricular pathways in patients with the symptom of disequilibrium. It may also be helpful in evaluating patients with certain auditory symptoms (such as hyperacusis, pulsatile tinnitus or autophony).
Diseases that may be diagnosed by this test
Diseases of the labyrinth and vestibular nerve are sometimes diagnosable if they involve utricular pathways.
Some lesions causing vestibular weakness may be detectable on oVEMPs if there is involvement of the utricle or its afferents through the vestibular nerve.
Third window phenomena, such as semicircular canal dehiscence, can manifest with abnormally large-amplitude ocular vestibular evoked myogenic potentials contralateral to the stimulated ear. Confidence in the diagnosis increases if the stimulated ear exhibits low oVEMP thresholds, and if audiometry on that side also shows conductive hyperacusis.
References
Agrawal Y, Zuniga MG, Davalos-Bichara M, Schubert MC, Walston JD, Hughes J, Carey JP (2012) Decline in semicircular canal and otolith function with age. Otol Neurotol 33: 832-9. doi: 10.1097/MAO.0b013e3182545061
Cengiz D, Demir İ, Çolak S, Demirel Birişik S, Karababa E, Bayindir T (2023) Effects of Gaze Position on Ocular Vestibular Evoked Myogenic Potential (oVEMP). Journal of Basic and Clinical Health Sciences 7: 337-344. doi: 10.30621/jbachs.1108971
Chihara Y, Iwasaki S, Ushio M, Murofushi T (2007) Vestibular-evoked extraocular potentials by air-conducted sound: another clinical test for vestibular function. Clin Neurophysiol 118: 2745-51. doi: 10.1016/j.clinph.2007.08.005
Dlugaiczyk J (2020) Evidence-based diagnostic use of VEMPs (Evidenzbasierte VEMP-Diagnostik): From neurophysiological principles to clinical application (Von den neurophysiologischen Grundlagen zur klinischen Anwendung). HNO. doi: 10.1007/s00106-019-00767-2
Fife TD, Colebatch JG, Kerber KA, Brantberg K, Strupp M, Lee H, Walker MF, Ashman E, Fletcher J, Callaghan B, Gloss DS, 2nd (2017) Practice guideline: Cervical and ocular vestibular evoked myogenic potential testing: Report of the Guideline Development, Dissemination, and Implementation Subcommittee of the American Academy of Neurology. Neurology 89: 2288-2296. doi: 10.1212/WNL.0000000000004690
Govender S, Rosengren SM, Colebatch JG (2009) The effect of gaze direction on the ocular vestibular evoked myogenic potential produced by air-conducted sound. Clin Neurophysiol 120: 1386-91. doi: 10.1016/j.clinph.2009.04.017
Jongkees LB, Maas JP, Philipszoon AJ (1962) Clinical nystagmography. A detailed study of electro-nystagmography in 341 patients with vertigo. Pract Otorhinolaryngol (Basel) 24: 65-93.
Kantner C, Gurkov R (2014) The effects of commonly used upward gaze angles on ocular vestibular evoked myogenic potentials. Otol Neurotol 35: 289-93. doi: 10.1097/MAO.0b013e318299a812
Miller EF, 2nd (1962) Counterrolling of the human eyes produced by head tilt with respect to gravity. Acta Otolaryngol 54: 479-501.
Murnane OD, Akin FW, Kelly KJ, Byrd S (2011) Effects of stimulus and recording parameters on the air conduction ocular vestibular evoked myogenic potential. J Am Acad Audiol 22: 469-80. doi: 10.3766/jaaa.22.7.7
Park HJ, Lee IS, Shin JE, Lee YJ, Park MS (2010) Frequency-tuning characteristics of cervical and ocular vestibular evoked myogenic potentials induced by air-conducted tone bursts. Clin Neurophysiol 121: 85-9. doi: 10.1016/j.clinph.2009.10.003
Piker EG, Jacobson GP, McCaslin DL, Hood LJ (2011) Normal characteristics of the ocular vestibular evoked myogenic potential. J Am Acad Audiol 22: 222-30. doi: 10.3766/jaaa.22.4.5
![]()